Video 1
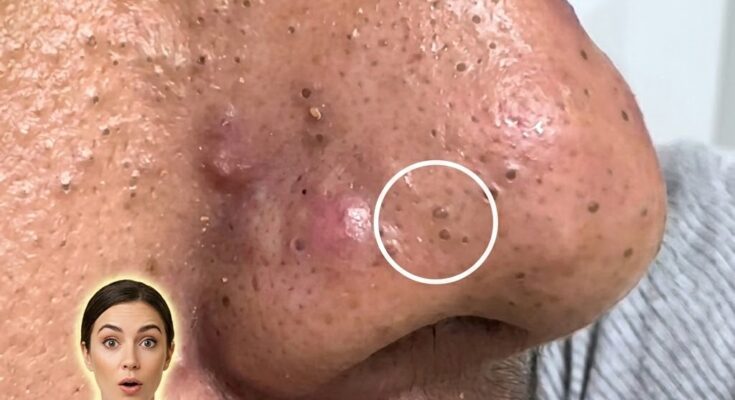
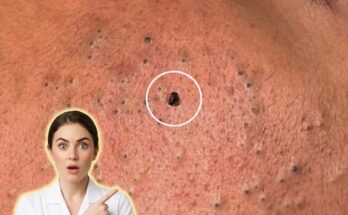
Clogged pores begin as a disruption in the normal process of skin cell turnover within the hair follicle. Under typical conditions, dead skin cells are shed gradually and carried to the surface along with sebum, the skin’s natural oil. When this process becomes irregular, excess keratinized cells accumulate and mix with sebum, forming a plug known as a comedone. At this stage, the pore may appear as a blackhead or whitehead and is not necessarily inflamed. However, when the follicle environment becomes favorable for the proliferation of acne-associated bacteria, particularly Cutibacterium acnes, the immune system may recognize this buildup as a threat. This triggers an inflammatory response, leading to redness, swelling, and tenderness in the surrounding skin.
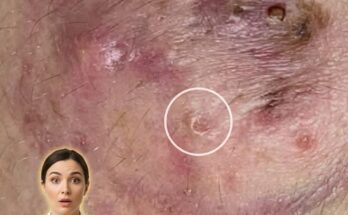
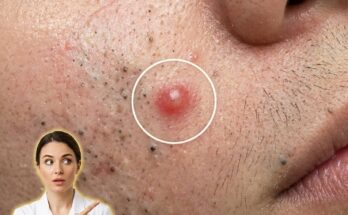
The transition from a simple clogged pore to a red, swollen lesion is largely driven by this immune activity. As bacteria break down trapped sebum, they release substances that can irritate the follicular wall. In response, the body sends immune cells to the area, increasing blood flow and causing visible redness. If the follicle wall becomes weakened or ruptures, its contents can spill into the surrounding tissue, intensifying inflammation and leading to papules or pustules. This process explains why some acne lesions feel painful or appear raised compared to non-inflamed comedones.
Several contributing factors can influence whether a clogged pore becomes inflamed. Hormonal fluctuations, particularly increases in androgens, can stimulate excess sebum production, creating an environment more prone to blockage and bacterial growth. Skincare habits also play a role, as the use of comedogenic products or inadequate cleansing may contribute to buildup within pores. Environmental factors such as humidity and pollution can further exacerbate oil production and skin congestion. Additionally, individual variations in immune response mean that some people are more prone to inflammation even with similar levels of pore blockage.
Management strategies often focus on both preventing clogged pores and reducing inflammation. Ingredients such as salicylic acid are commonly used to penetrate into pores and help dissolve excess sebum and dead skin cells. Retinoids are often recommended for their ability to normalize skin cell turnover and prevent the formation of new comedones. Benzoyl peroxide may help reduce acne-causing bacteria and limit inflammatory responses, while niacinamide is frequently used to support the skin barrier and calm redness. For more persistent or severe inflammatory acne, dermatology treatments such as prescription retinoids, topical or oral antibiotics, or other targeted therapies may be considered.
It is important to recognize that not all clogged pores will become inflamed, and the progression can vary depending on individual skin biology and external factors. Consistent skincare practices and early intervention may help reduce the likelihood of redness and swelling, but results are typically gradual rather than immediate. Individuals experiencing frequent or severe inflammatory acne are generally advised to seek guidance from a qualified dermatology professional to ensure appropriate and safe treatment.