Video 1
Video 2
Video 3
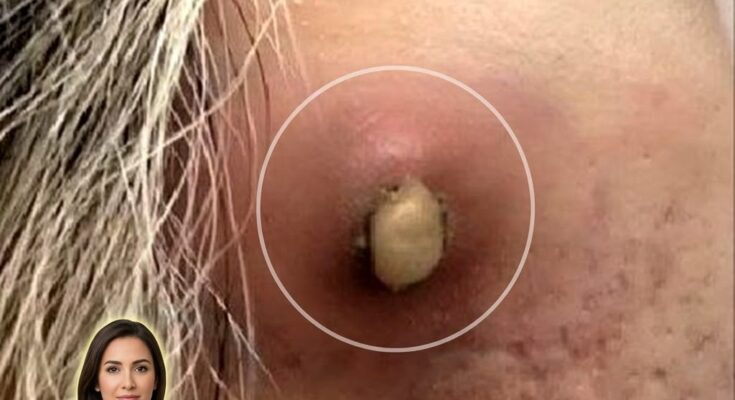
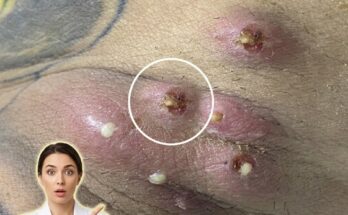
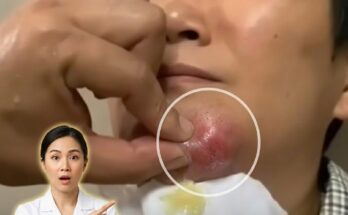
Comedonal acne develops when hair follicles become clogged with a mixture of excess sebum and dead skin cells. In healthy skin, keratinocytes inside the follicle naturally shed and move outward through the pore. In acne-prone skin, this shedding process can become irregular, leading to a buildup of keratinized cells that combine with sebum and form a plug. These plugs create comedones, which appear as blackheads when the pore remains open and whiteheads when the pore becomes closed beneath the skin surface. Dermatology research has shown that abnormal follicular keratinization is one of the earliest steps in acne development, which is why treatments that normalize this process are often central to acne care.
Retinoids are commonly used for comedonal acne because they influence the way skin cells grow and shed within the follicle. Derived from vitamin A, retinoids interact with receptors in skin cells that regulate cellular turnover. By encouraging more consistent shedding of keratinocytes, these medications help reduce the buildup of dead skin cells that contribute to clogged pores. Over time, this process may help prevent the formation of new comedones while also gradually clearing existing blockages inside the follicles.
Several factors can contribute to the development of comedonal acne, which is why retinoids are often used as part of a broader treatment approach. Hormonal fluctuations may stimulate the sebaceous glands to produce more oil, particularly during puberty, menstrual cycles, or periods of hormonal imbalance. Increased sebum production can combine with sticky skin cells inside the follicle, creating an environment where plugs form more easily. Certain skincare habits may also influence pore congestion. Heavy or occlusive cosmetic products, inconsistent cleansing routines, or harsh exfoliation that disrupts the skin barrier may contribute to conditions that favor clogged pores.
Environmental factors may also play a role in comedonal acne. Humidity, air pollution, and friction from helmets, masks, or tight clothing can influence how the skin behaves and how pores become obstructed. Genetic tendencies may further affect how strongly a person’s skin produces sebum or how quickly skin cells accumulate inside follicles. Because these factors interact in complex ways, dermatologists often focus on treatments that address the underlying biology of pore blockage rather than only the visible lesions.
Topical retinoids are frequently recommended as a first-line therapy for comedonal acne in dermatology guidelines. Over-the-counter retinoid options such as adapalene are widely used in skincare routines, while prescription retinoids like tretinoin, tazarotene, or trifarotene may be recommended for individuals with more persistent or widespread acne. These treatments are typically applied at night and are often introduced gradually to reduce irritation while the skin adapts.
Retinoids are also commonly combined with other acne treatments that target different aspects of the acne process. Ingredients such as salicylic acid may help dissolve oil and debris within pores, while benzoyl peroxide is often used to reduce acne-causing bacteria and inflammation. Niacinamide is another ingredient frequently included in acne-focused skincare formulations because it may help support the skin barrier and regulate oil production. When used together under appropriate guidance, these treatments can address multiple contributors to acne formation.
Although retinoids are widely used in acne management, it is important to recognize that results typically develop gradually. Because these medications influence the skin’s renewal cycle, visible improvements often appear over several weeks to months as clogged pores slowly clear and new blockages become less common. Mild dryness, peeling, or irritation may occur during the early stages of treatment, which is why dermatologists often recommend gentle cleansers, non-comedogenic moisturizers, and sun protection as supportive skincare practices.
Comedonal acne can vary widely in severity and persistence, and individual responses to treatment may differ. For people experiencing ongoing or severe acne, consultation with a qualified dermatologist can help determine the most appropriate treatment plan and ensure that medications are used safely and effectively. Evidence-based skincare strategies that focus on normalizing pore function, reducing excess oil, and maintaining skin barrier health remain central to long-term acne management.