Video 1
Video 2
Video 3
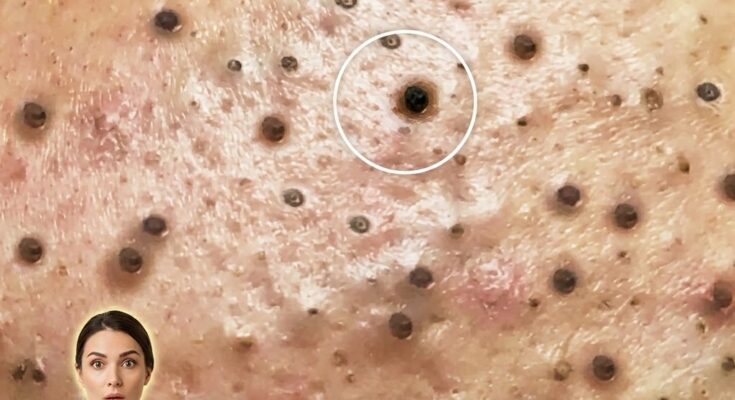
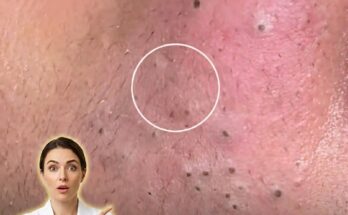
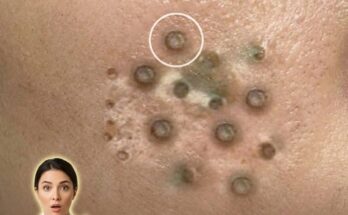
Hydration plays a fundamental role in maintaining normal skin function, particularly in how the skin barrier operates and how pores behave. The outermost layer of the skin, known as the stratum corneum, relies on an appropriate balance of water and lipids to remain flexible, intact, and protective. When hydration levels are adequate, this layer helps regulate transepidermal water loss while supporting enzymatic processes involved in natural exfoliation. When hydration is compromised, the skin barrier may become less efficient, leading to increased water loss, surface roughness, and a tendency for dead skin cells to accumulate within pores.
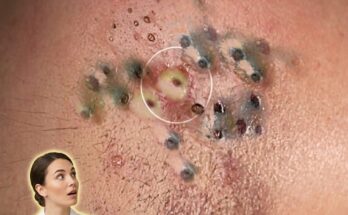
This accumulation of corneocytes can contribute to follicular keratinization, a key step in the formation of comedones such as blackheads and whiteheads. In dehydrated skin, impaired shedding of dead skin cells may combine with sebum to form plugs within the follicle. At the same time, the skin may respond to dehydration by increasing oil production in an attempt to compensate for barrier disruption. This combination of excess sebum and retained keratin can create an environment where clogged pores and acne lesions are more likely to develop.
Hydration is also closely linked to inflammation and skin sensitivity. A weakened skin barrier may allow external irritants, pollutants, and microbes to penetrate more easily, potentially triggering inflammatory responses. This can worsen existing acne or make the skin more reactive to treatments. In addition, dehydration may affect the skin microbiome, which plays a role in maintaining balance within the follicle and regulating acne-related bacteria.
Several factors can influence skin hydration, including environmental conditions such as low humidity, excessive sun exposure, and frequent use of harsh cleansers or exfoliants. Skincare habits that strip the skin of its natural lipids, such as overuse of strong foaming cleansers or alcohol-based products, may further impair hydration levels. Internal factors, including hormonal fluctuations and individual skin type, can also affect how well the skin retains moisture.
From a treatment perspective, maintaining hydration is often considered a supportive strategy in acne management. Non-comedogenic moisturizers containing ingredients such as glycerin, hyaluronic acid, and ceramides may help improve water retention and reinforce the skin barrier. These ingredients support the skin’s ability to maintain balance without contributing to pore congestion. Niacinamide is also commonly used for its potential to enhance barrier function and regulate oil production.
At the same time, established acne treatments such as topical retinoids, salicylic acid, and benzoyl peroxide remain central to addressing clogged pores and inflammation. However, these treatments can sometimes cause dryness or irritation, which may worsen barrier function if not managed properly. Incorporating appropriate hydration alongside these treatments may improve tolerability and help maintain overall skin stability.
Professional dermatological treatments may also consider hydration as part of a broader approach. Procedures such as chemical peels or laser therapies are often paired with barrier-repair strategies to support recovery and reduce irritation. This highlights the importance of viewing hydration not as a standalone solution, but as a foundational component of overall skin health.
It is important to recognize that while proper hydration may support skin function and reduce some contributing factors to acne, it is not a cure for acne itself. Persistent or severe acne may require targeted medical treatments and evaluation by a qualified professional. A balanced approach that includes both active treatments and barrier-supportive care is generally considered the most effective strategy for long-term skin management.