Acne often begins during puberty because of biological changes that affect how the skin produces oil and how hair follicles function.
During this stage of development, the body increases production of androgen hormones, including testosterone and related compounds.
These hormones stimulate the sebaceous glands in the skin, causing them to enlarge and produce greater amounts of sebum,
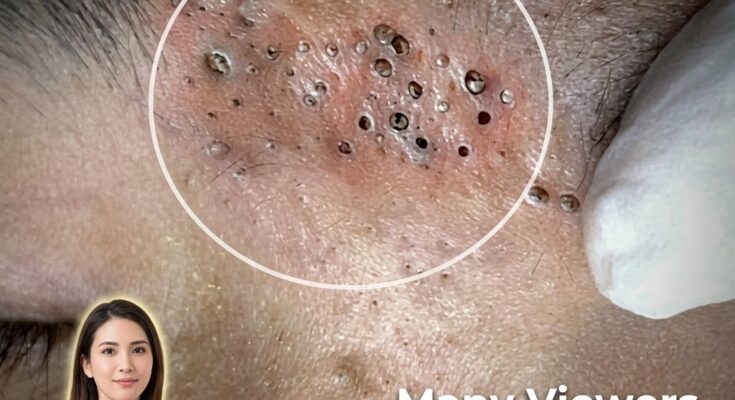
the oily substance that helps lubricate the skin and hair. When excess sebum mixes with dead skin cells inside the hair follicle, it can contribute to follicular keratinization, a process where shed skin cells do not exit the pore normally. This combination can lead to clogged pores and the formation of comedones, which appear as blackheads or whiteheads and are often the earliest visible signs of acne.
The increase in sebum production during puberty also creates an environment that may support the growth of bacteria naturally present on the skin, particularly Cutibacterium acnes. While this microorganism is a normal part of the skin microbiome, higher oil levels and blocked follicles may allow it to multiply more easily. The immune system can react to this buildup within the pore, which may trigger inflammation and lead to red or swollen acne lesions. For many adolescents, this sequence of increased oil production, clogged pores, and inflammation explains why acne commonly begins around the same time that other hormonal changes of puberty occur.
Genetics can also influence how strongly the skin responds to hormonal changes. Individuals with a family history of acne may have sebaceous glands that are more sensitive to androgen stimulation, which can result in higher sebum output and a greater tendency toward clogged pores. Environmental factors and daily habits may also play a role. Humid climates, certain cosmetics, and heavy or occlusive skincare products can sometimes contribute to pore blockage, particularly in individuals who already have oily or acne-prone skin. In addition, inconsistent cleansing habits or overly harsh skincare routines may disrupt the skin barrier, which can further influence inflammation and breakouts.
Evidence-informed skincare approaches often focus on addressing the biological processes involved in acne development. Ingredients such as salicylic acid are commonly used because they are oil-soluble and may help exfoliate inside the pore, supporting the removal of excess sebum and dead skin cells that contribute to blackheads and whiteheads. Retinoids are frequently recommended in dermatology because they help regulate skin cell turnover and may reduce the formation of new comedones. Benzoyl peroxide is another widely used treatment that can reduce acne-causing bacteria and may help limit inflammatory lesions when used appropriately. Supporting the skin barrier with gentle cleansers and non-comedogenic moisturizers is also often encouraged, as maintaining balanced skin can reduce irritation that may worsen acne.
Some individuals may also benefit from skincare ingredients that help regulate oil production or calm inflammation. Niacinamide, for example, is commonly included in acne-focused formulations because it may help support barrier function and improve the appearance of oily skin. Consistent skincare routines are generally emphasized in acne management, as the biological processes that lead to clogged pores occur continuously over time. Dermatologists may also recommend prescription treatments, including topical retinoids, oral medications, or hormonal therapies, for individuals with persistent or more severe acne.
Although acne during puberty is extremely common, it can vary widely in severity and duration. Many people experience gradual improvement as hormone levels stabilize over time, while others may continue to have acne into adulthood. Treatment often requires patience because the skin cycle takes several weeks, meaning visible improvements may develop gradually. Individuals experiencing persistent, painful, or scarring acne are often encouraged to seek evaluation from a qualified dermatology professional who can recommend treatments tailored to their skin type and medical history. Educational, evidence-based skincare strategies can play an important role in managing acne safely while supporting overall skin health.