Video 1
Video 2
Video 3
Acne develops through a series of tightly regulated cellular processes within the pilosebaceous unit, which consists of the hair follicle and its associated sebaceous gland. At the cellular level, the condition begins with an overproduction of sebum by sebocytes, the specialized cells that produce skin oils. These cells respond strongly to androgens, particularly dihydrotestosterone, which can increase both the size and activity of sebaceous glands. As sebum accumulates, it mixes with dead skin cells that are shed from the follicular lining, creating an environment where normal shedding becomes disrupted and leads to retention of keratinocytes within the pore.
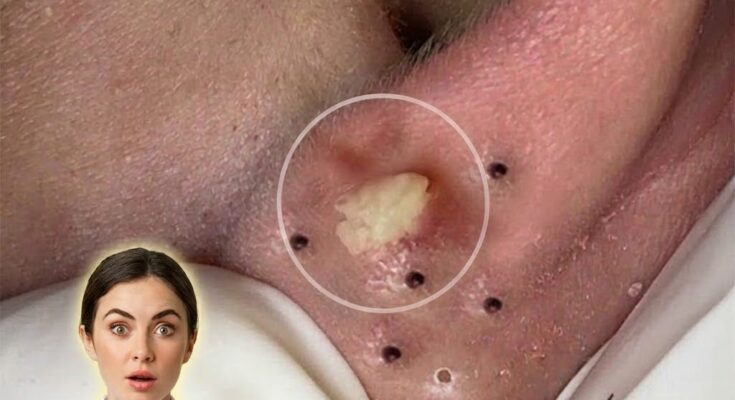
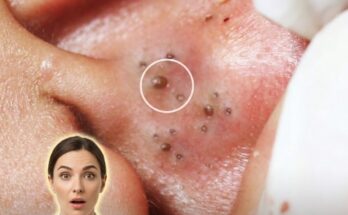
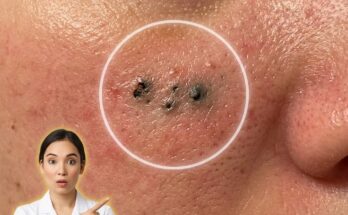
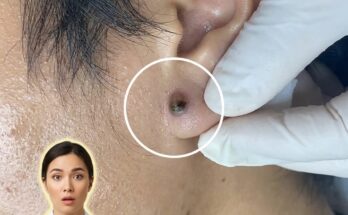
A key mechanism in acne formation is abnormal follicular keratinization. Under normal conditions, keratinocytes within the follicle mature and shed in a controlled manner. In acne-prone skin, this process becomes dysregulated, leading to cohesion between dead cells and the formation of a dense plug known as a microcomedone. This microscopic blockage is considered the earliest visible stage of acne and can later develop into blackheads or whiteheads depending on whether the pore remains open or becomes fully closed. These structural changes are driven by altered cell signaling, including increased proliferation and reduced desquamation of keratinocytes.
As the follicle becomes clogged, the lipid-rich and oxygen-poor environment favors the growth of Cutibacterium acnes, a bacterium that naturally resides on the skin. At the cellular level, this bacterium interacts with immune cells such as keratinocytes and macrophages, triggering the release of pro-inflammatory cytokines. These signaling molecules, including interleukin-1 and tumor necrosis factor-alpha, initiate an inflammatory cascade that contributes to redness, swelling, and the formation of papules and pustules. The immune response is not solely due to bacterial presence but also to the breakdown products of sebum, which can act as inflammatory stimuli.
Inflammation in acne is increasingly understood to begin even before visible lesions form. Early activation of innate immune pathways can alter the behavior of surrounding skin cells, further disrupting barrier function and amplifying the cycle of blockage and irritation. Oxidative stress within the follicle may also play a role, as lipid peroxidation of sebum components can increase inflammatory signaling and damage nearby cells. This helps explain why acne is not simply a surface issue but a complex interaction between skin cells, immune responses, and microbial activity.
Several contributing factors can influence these cellular processes. Hormonal fluctuations, particularly during puberty or periods of endocrine imbalance, can increase sebocyte activity and sebum production. Genetic predisposition may affect how skin cells respond to hormones or regulate keratinization. Environmental factors such as humidity, occlusive skincare products, and pollution may alter pore behavior and contribute to congestion. Skincare habits, especially the use of heavy or comedogenic formulations, can exacerbate follicular blockage, while over-cleansing or harsh treatments may impair the skin barrier and increase inflammation .
Treatment approaches often target these cellular mechanisms to reduce acne development. Retinoids are commonly recommended because they normalize keratinocyte turnover and help prevent microcomedone formation. Salicylic acid penetrates into the pore and supports the breakdown of accumulated debris, making it useful for managing blackheads and whiteheads. Benzoyl peroxide works by reducing bacterial load and has anti-inflammatory effects, while niacinamide may help regulate sebum production and support the skin barrier. In more persistent cases, dermatological treatments such as oral medications or procedural therapies may be considered to address deeper inflammatory pathways.
Understanding acne at the cellular level highlights why consistent and balanced skincare is important. Improvements typically occur gradually as cellular turnover cycles normalize, which can take several weeks. Overly aggressive treatments may disrupt the skin barrier and worsen inflammation, so a measured approach is generally advised. Individuals experiencing moderate to severe or persistent acne are often encouraged to seek guidance from a qualified dermatology professional to ensure appropriate and safe management.