The world of plants is a vibrant tapestry of life, intricately woven into the fabric of our daily existence.
From the towering trees that grace our forests to the delicate flowers that bloom in our gardens, plants play a crucial role in sustaining life on Earth.
Their fascinating journey, filled with resilience and adaptability, invites us to look closer at the incredible ways they enrich our lives.
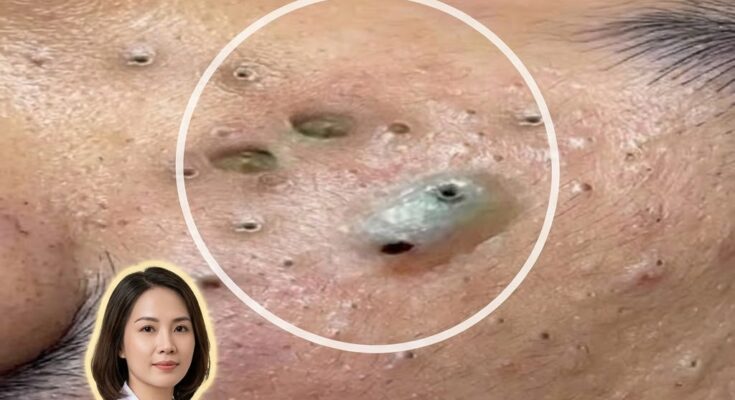
Post-inflammatory hyperpigmentation (PIH) is a common skin response that can appear after inflammatory acne lesions heal. It occurs when the skin produces excess melanin during the healing process following inflammation in the hair follicle. Acne begins within the pilosebaceous unit, where increased sebum production, follicular keratinization, and the accumulation of dead skin cells can lead to clogged pores and the formation of comedones such as blackheads and whiteheads. When a clogged pore becomes inflamed, immune signaling molecules are released in the surrounding skin. These inflammatory mediators can stimulate melanocytes, the pigment-producing cells in the epidermis, leading them to increase melanin production. As the skin repairs the damaged tissue, the excess pigment may remain in the area, creating flat dark marks that persist after the acne lesion itself has resolved.
The likelihood of developing post-inflammatory hyperpigmentation often depends on the intensity and duration of the inflammation within the pore. Deeper inflammatory lesions such as papules, pustules, or nodules may produce stronger immune responses, which can increase melanocyte activity. Skin types with higher baseline melanin levels may also be more prone to visible hyperpigmentation because melanocytes are naturally more active. In addition, prolonged irritation of the skin barrier may amplify inflammatory signaling. When the barrier becomes compromised, the skin may respond with increased sensitivity and pigment production during the healing process.
Several everyday factors can influence how often PIH appears after acne. Hormonal fluctuations that increase sebum production may contribute to recurring breakouts, which can lead to repeated cycles of inflammation and pigmentation. Skincare habits also play a role. Aggressive scrubbing, picking at acne lesions, or using overly harsh treatments may worsen inflammation within the follicle and surrounding skin. Environmental factors such as ultraviolet exposure can further stimulate melanocytes, potentially darkening existing marks and prolonging the visibility of pigmentation after acne has healed.
Many acne management strategies aim to reduce both pore congestion and inflammation, which may indirectly help lower the risk of post-inflammatory hyperpigmentation. Ingredients commonly used in acne skincare include salicylic acid, which can help dissolve excess oil and dead skin cells within pores, and benzoyl peroxide, which is often used to reduce acne-causing bacteria and inflammatory activity. Retinoids are frequently recommended in dermatology because they help normalize skin cell turnover within the follicle, which may reduce the formation of clogged pores and comedones. By limiting repeated inflammation in the skin, these treatments may reduce the likelihood of new pigmentation marks developing.
Certain skincare ingredients are also used specifically to help improve the appearance of existing hyperpigmentation. Niacinamide is commonly included in formulations designed for acne-prone skin because it may help support the skin barrier and regulate oil production while also influencing pigment distribution within the skin. Consistent use of broad-spectrum sunscreen is also considered important, as ultraviolet radiation can intensify melanocyte activity and make dark marks more persistent. In some cases, dermatologists may recommend prescription-strength retinoids, azelaic acid, or chemical exfoliants to gradually encourage more even skin tone as the skin renews itself.
It is important to recognize that post-inflammatory hyperpigmentation often fades gradually as normal skin turnover replaces pigmented cells with new ones. However, this process can take several weeks to months depending on the depth of pigment in the skin and the individual’s skin type. Because aggressive treatments may irritate the skin barrier and potentially worsen pigmentation, many dermatology professionals emphasize gentle skincare routines and consistent acne management. Individuals experiencing persistent or severe pigmentation after acne may benefit from consulting a qualified dermatology professional who can recommend personalized treatment options based on their skin type and acne history.
The development and management of post-inflammatory hyperpigmentation is closely connected to the broader biological processes involved in acne formation, including sebum production, follicular blockage, microbial activity, and inflammation within the pore. Educational approaches to skincare often emphasize understanding these mechanisms so that treatment strategies can focus not only on clearing acne lesions but also on minimizing the long-term skin changes that may follow inflammation.