Exploring the World of Microorganisms
In the vast tapestry of life on Earth, there exists a hidden realm that is both intriguing and essential: the world of microorganisms.
These tiny organisms, often invisible to the naked eye, play an enormous role in our ecosystems, our health, and our daily lives.
As we dive into this microscopic universe, we can discover the beauty and complexity of life at a scale we often overlook.
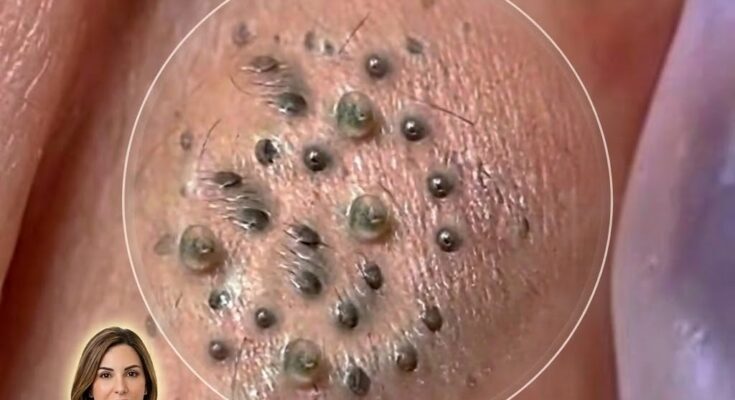
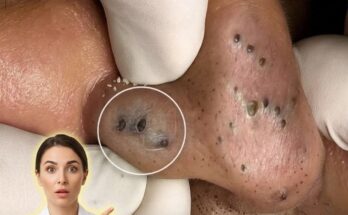
Acne often begins long before a visible pimple appears on the skin. One of the earliest microscopic events in the acne process is the formation of a microcomedone. A microcomedone is a tiny blockage that develops inside the hair follicle when excess oil and skin cells accumulate together. Although it cannot be seen with the naked eye, this small structure is widely considered the starting point of many types of acne lesions, including blackheads, whiteheads, and inflammatory breakouts. Understanding how microcomedones form can help explain why acne develops and why certain treatments focus on preventing clogged pores. Inside each pore is a hair follicle connected to a sebaceous gland that produces sebum, the natural oil that helps lubricate and protect the skin. Normally, dead skin cells shed gradually from the lining of the follicle and rise to the surface. In acne-prone skin, this shedding process may become irregular. Instead of separating cleanly, the cells may stick together and mix with sebum inside the follicle. This combination forms a plug known as follicular hyperkeratinization. At the microscopic level, this plug is called a microcomedone.
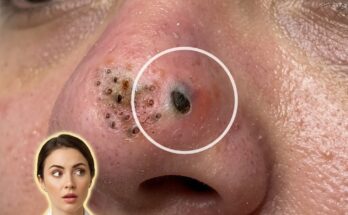
As the microcomedone grows, it can gradually enlarge and evolve into a visible comedone. If the follicle remains closed at the surface, the trapped material appears as a whitehead. If the follicle opening widens and the contents are exposed to air, oxidation of sebum and melanin can cause the dark appearance associated with blackheads. These visible lesions are often the first signs people notice, even though the biological process began earlier beneath the skin.
Several internal and external factors may influence how frequently microcomedones form. Hormonal fluctuations, particularly increases in androgens, can stimulate sebaceous glands to produce more oil. Higher levels of sebum may make it easier for dead skin cells to accumulate and clog the follicle. Genetics may also influence pore size, sebum production, and the tendency toward retention of keratin within the follicle, which may explain why acne tends to run in families.
Environmental factors and skincare habits can also contribute to pore congestion. Heavy or highly occlusive skincare products may increase the likelihood of buildup inside pores for some individuals, particularly those with oily skin. Inadequate cleansing or inconsistent removal of sunscreen and makeup may allow residue to remain on the skin surface, which can interact with natural oils and contribute to clogged pores over time. At the same time, excessive cleansing or harsh exfoliation may disrupt the skin barrier and increase irritation, which can worsen acne in certain cases.
Bacteria that naturally live on the skin also play a role in the progression of microcomedones. The follicle provides an environment where Cutibacterium acnes may grow more easily when sebum accumulates. As these bacteria interact with trapped oil and cellular debris, inflammatory signals may develop within the follicle. This process can eventually transform a non-inflamed comedone into a red or painful inflammatory lesion.
Because microcomedones form beneath the surface, many acne treatments are designed to prevent their development rather than simply treating visible pimples. Topical retinoids are widely used in dermatology because they help normalize skin cell turnover and reduce the formation of follicular plugs. Ingredients such as salicylic acid may help exfoliate within the pore and dissolve some of the oil and debris that contribute to congestion. Benzoyl peroxide is often recommended when inflammatory acne is present because it helps reduce acne-associated bacteria and may decrease inflammation within the follicle.
Other skincare ingredients may support acne-prone skin by addressing contributing factors. Niacinamide is commonly included in formulations designed for oily or acne-prone skin because it may help regulate sebum production and support the skin barrier. Lightweight moisturizers labeled as non-comedogenic are frequently recommended to maintain hydration without heavily occluding pores, which may help reduce irritation from acne treatments.
Even with appropriate skincare, microcomedones can continue to form because acne is influenced by many biological factors. For individuals with persistent or moderate to severe acne, dermatologists may recommend prescription retinoids, topical or oral antibiotics, hormonal treatments, or other medical therapies depending on the underlying cause and severity of the condition. Professional guidance can help determine which treatment approach is most appropriate.
Understanding microcomedones highlights why acne management often focuses on long-term prevention rather than quick fixes. Because these early blockages form beneath the skin weeks before a breakout becomes visible, consistent skincare and patience are important when evaluating treatments. Many therapies require several weeks or months before noticeable improvement occurs, and professional medical advice may be helpful when acne becomes persistent, severe, or resistant to over-the-counter approaches.