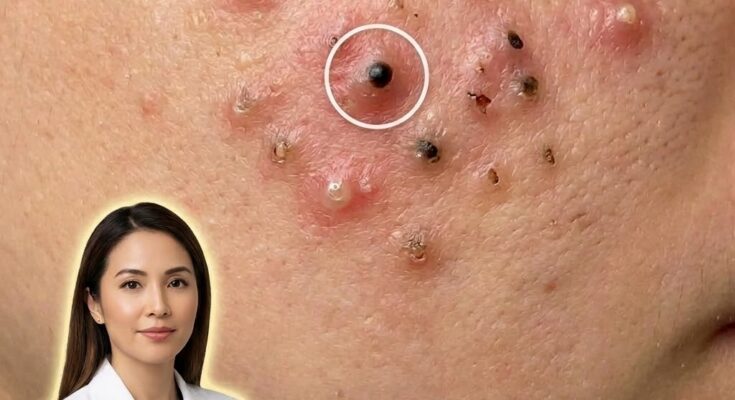
Acne development is closely linked to biological processes occurring within the hair follicle,
where oil glands produce sebum that helps lubricate and protect the skin.
When excess sebum mixes with dead skin cells inside the follicle,
the pore can become clogged, creating an environment that supports the growth of acne-associated bacteria known as Cutibacterium acnes. Benzoyl peroxide is widely used in dermatology because it directly targets this microbial component of acne formation. When applied to the skin, benzoyl peroxide breaks down and releases oxygen within the pore. Since C. acnes thrives in low-oxygen environments, the increased oxygen levels can reduce bacterial growth. This antibacterial effect may help decrease the inflammatory signals that contribute to red, swollen acne lesions.
In addition to its antibacterial activity, benzoyl peroxide also influences several other steps involved in acne development. The ingredient has mild keratolytic properties, meaning it can help loosen and remove dead skin cells that accumulate around the follicle opening. This process may reduce the formation of clogged pores that lead to comedones such as blackheads and whiteheads. By addressing both bacterial activity and pore blockage, benzoyl peroxide is commonly used as part of broader acne treatment strategies that target multiple factors in the acne cycle, including excess oil production, follicular keratinization, and inflammation.
Several internal and external influences can contribute to the conditions that allow acne bacteria to thrive. Hormonal fluctuations, particularly those involving androgens, can increase sebum production within the sebaceous glands. Increased oil levels may create a richer environment for bacterial growth and pore blockage. Genetic predisposition may also influence how active sebaceous glands are and how quickly skin cells shed inside the follicle. Environmental factors such as humidity, occlusive cosmetics, or heavy skincare products may further contribute to clogged pores in individuals with oily or acne-prone skin.
Skincare habits also play an important role in how effectively treatments like benzoyl peroxide work. Overwashing or using harsh cleansers can disrupt the skin barrier, potentially increasing irritation and inflammation. On the other hand, consistent use of gentle cleansing and non-comedogenic moisturizers may help maintain barrier function while supporting acne treatments. Ingredients such as salicylic acid are often used alongside benzoyl peroxide because they help dissolve oil and debris inside pores, while topical retinoids can promote more regular skin cell turnover. This combination approach reflects the understanding that acne rarely results from a single cause.
Benzoyl peroxide is available in a variety of over-the-counter formulations, including cleansers, gels, creams, and spot treatments with concentrations typically ranging from 2.5 percent to 10 percent. Lower concentrations are often recommended initially because they may provide similar antibacterial benefits while reducing the likelihood of irritation. Dermatologists sometimes incorporate benzoyl peroxide into prescription treatment plans as well, frequently combining it with topical antibiotics or retinoids to improve overall acne management and reduce bacterial resistance.
Despite its effectiveness, benzoyl peroxide can cause dryness, redness, or peeling in some individuals, particularly when first introduced into a skincare routine. Gradual use and proper moisturizing may help the skin adjust over time. It is also known to bleach fabrics, which is why dermatology guidance often recommends caution with clothing and bedding during treatment. Individuals with persistent, severe, or scarring acne are generally encouraged to seek evaluation from a qualified healthcare professional who can determine whether additional therapies may be appropriate.
Understanding the role of acne bacteria provides insight into why ingredients like benzoyl peroxide remain a cornerstone of many acne treatment strategies. By helping reduce bacterial activity within clogged pores while also supporting the removal of dead skin cells, this ingredient addresses several biological mechanisms involved in acne formation. However, long-term improvement typically depends on consistent skincare habits, individualized treatment plans, and realistic expectations about how gradually the skin responds to therapy. Educational dermatology resources emphasize that acne management often requires patience and ongoing adjustment of treatment approaches as the skin changes over time.