Video 1
Video 2
Video 3
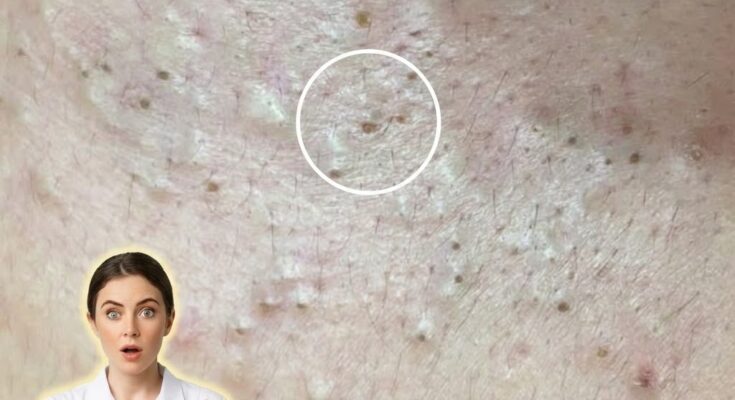
The skin microbiome refers to the diverse community of microorganisms, including bacteria, fungi, and viruses, that naturally reside on the skin’s surface. This ecosystem plays an essential role in maintaining skin barrier function, regulating inflammation, and supporting immune responses. In the context of acne, the microbiome is closely linked to processes such as sebum production, follicular keratinization, and the formation of clogged pores. One of the most studied bacteria in acne is Cutibacterium acnes, which is a normal resident of the skin but can contribute to inflammation when its balance within the microbiome is disrupted. Rather than the mere presence of this bacterium, it is often the shift in microbial diversity and activity that influences whether acne develops or worsens.
The composition of the skin microbiome can be affected by multiple internal and external factors. Hormonal fluctuations, particularly increases in androgens, can stimulate excess sebum production, creating an environment where certain bacteria may thrive. Skincare habits also play a significant role, as over-cleansing, harsh exfoliation, or frequent use of strong antibacterial products may disrupt the natural microbial balance. Environmental influences such as humidity, pollution, and occlusive cosmetic formulations can further alter the microbiome, potentially contributing to pore congestion and the development of blackheads and whiteheads. Genetic predisposition may also influence how an individual’s immune system responds to microbial changes, affecting inflammation levels and acne severity.
When the microbiome becomes imbalanced, a state sometimes referred to as dysbiosis, the skin may become more prone to inflammation and barrier dysfunction. This can lead to increased sensitivity, impaired healing, and a higher likelihood of developing inflammatory acne lesions. Additionally, disruptions in the microbiome may influence how skin cells shed داخل the pore lining, contributing to the buildup of dead skin cells and sebum that form comedones. Maintaining a stable and diverse microbiome is therefore considered an important factor in supporting clearer skin.
Treatment approaches often aim to manage acne while preserving or restoring microbial balance. Ingredients such as benzoyl peroxide are commonly used to reduce acne-causing bacteria, although they may also affect beneficial microbes. Retinoids are frequently recommended because they help normalize follicular keratinization and prevent clogged pores without directly targeting bacteria. Salicylic acid, an oil-soluble exfoliant, can penetrate pores to dissolve excess sebum and debris, which may indirectly support a healthier microbiome by reducing the conditions that promote bacterial overgrowth. Niacinamide is another ingredient often included in skincare routines, as it may help regulate oil production, support the skin barrier, and reduce inflammation.
Emerging research has also explored the role of prebiotics, probiotics, and microbiome-friendly skincare formulations. These approaches aim to support beneficial microorganisms rather than eliminate bacteria entirely, although more long-term clinical evidence is still developing. Gentle cleansing routines, avoidance of over-exfoliation, and the use of non-comedogenic products are generally recommended to help maintain microbial balance while managing acne symptoms.
It is important to recognize that acne is a multifactorial condition, and the skin microbiome is only one component among many contributing factors. While supporting microbial balance may help improve overall skin health, results can vary depending on individual skin type, hormonal influences, and the severity of acne. Persistent or severe cases may require evaluation by a qualified dermatologist, who can recommend appropriate treatments tailored to the individual. Maintaining realistic expectations and focusing on consistent, evidence-based skincare practices can support long-term skin health and reduce the risk of further irritation or imbalance