Chemistry is often viewed as a complicated and abstract science, but in reality, it plays a fundamental role in our everyday lives, shaping the materials we encounter regularly.
From the clothes we wear to the food we eat and the products we use in our homes, chemistry is the invisible thread that weaves through our daily existence.
By understanding how chemistry influences these materials, we can appreciate the intricate balance of nature and innovation that surrounds us.
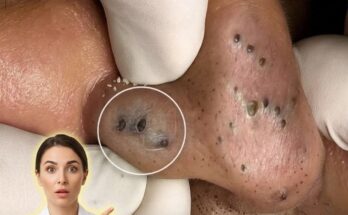
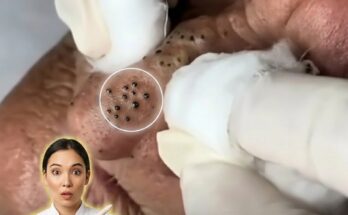
Inflammatory acne breakouts develop through a complex interaction between excess oil production, clogged pores, and the activity of skin-dwelling bacteria. One of the most important microorganisms involved in this process is Cutibacterium acnes, a bacterium that normally lives within hair follicles and pores as part of the skin’s natural microbiome. Under typical conditions it coexists harmlessly with the skin. However, when pores become blocked by a mixture of sebum and dead skin cells, the environment inside the follicle can change in ways that allow this bacterium to contribute to inflammation and the development of acne lesions.
Acne formation often begins with increased sebum production from sebaceous glands. Hormonal signals, particularly androgens, can stimulate these glands to produce more oil, which mixes with keratinized skin cells inside the pore. When this mixture accumulates faster than it can exit the follicle, it may form a microcomedone, the earliest stage of a clogged pore. Within this oil-rich and oxygen-limited environment, Cutibacterium acnes can multiply more rapidly. The bacterium produces enzymes known as lipases that break down sebum into fatty acids, which may irritate the follicular wall and contribute to inflammatory signaling within the skin.
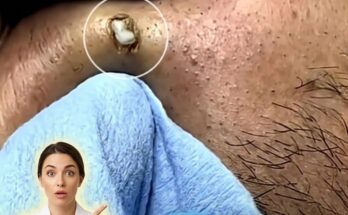
As the bacterial population increases inside the clogged follicle, the immune system may recognize bacterial components and metabolic byproducts as potential threats. This immune response can trigger the release of inflammatory molecules such as cytokines. Inflammation can weaken the follicular wall and allow its contents—including oil, keratin debris, and bacteria—to leak into surrounding skin tissue. When this occurs, the body’s immune system responds more aggressively, leading to the visible redness, swelling, and tenderness commonly associated with inflammatory acne lesions such as papules and pustules.
Several factors can influence how strongly Cutibacterium acnes contributes to inflammatory breakouts. Hormonal fluctuations may increase sebum production and make pores more prone to clogging, while genetics can affect both oil gland activity and inflammatory sensitivity. Skincare habits may also play a role. Heavy or occlusive products can sometimes contribute to pore congestion in acne-prone individuals, while over-exfoliation may disrupt the skin barrier and increase irritation. Environmental factors such as humidity, sweat, and friction from clothing or masks may also create conditions that encourage clogged pores and bacterial activity.
Because inflammation is closely tied to both bacterial activity and pore blockage, many acne treatments focus on addressing these underlying mechanisms. Ingredients such as benzoyl peroxide are commonly used because they can reduce the population of acne-associated bacteria within pores while also helping limit inflammatory activity. Salicylic acid, a beta hydroxy acid, is often recommended for oily or acne-prone skin because it penetrates into pores and helps dissolve excess oil and dead skin cells that contribute to comedones. Topical retinoids are frequently used in dermatology because they help normalize follicular keratinization, which may reduce the formation of clogged pores where bacteria can thrive.
Other supportive ingredients may help calm the surrounding skin environment. Niacinamide is widely used in skincare formulations because it may help regulate oil production, support the skin barrier, and reduce visible redness associated with inflammation. Gentle cleansing routines and non-comedogenic moisturizers may also support overall skin balance and help reduce factors that contribute to persistent clogged pores and breakouts.
Although Cutibacterium acnes plays a key role in inflammatory acne, it is important to recognize that acne is a multifactorial condition rather than a simple bacterial infection. Oil production, follicular keratinization, immune responses, hormones, and environmental influences all interact within the skin. As a result, effective acne management often involves a combination of consistent skincare practices and, in some cases, medical treatments recommended by dermatology professionals.
With appropriate care, many people can gradually improve the frequency and severity of inflammatory breakouts. However, deeper or persistent acne may require professional evaluation to prevent long-term inflammation or potential scarring. A qualified healthcare professional can help determine which treatments are most appropriate based on an individual’s skin type, acne severity, and overall skin health. Educational skincare guidance and evidence-based treatment strategies remain important components of managing acne and maintaining healthier pores over time.