Video 1
Video 2
Video 3
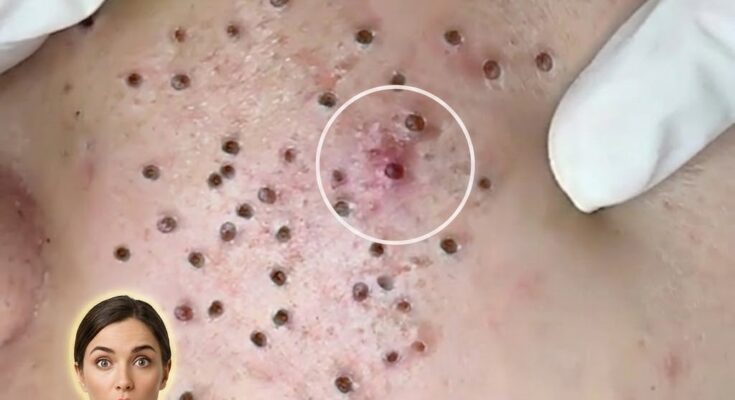
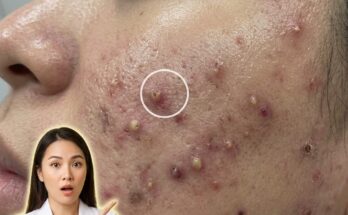
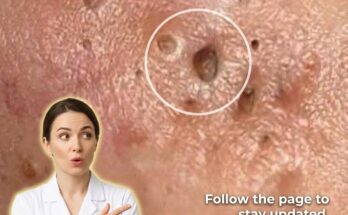
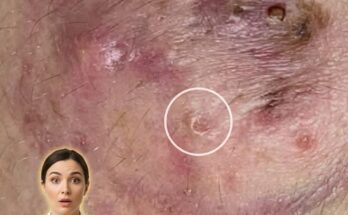
High glycemic foods are thought to influence acne development through their effects on hormones and skin physiology, particularly insulin and insulin-like growth factor 1 (IGF-1). When foods with a high glycemic index are consumed, such as refined carbohydrates and sugary snacks, they are rapidly broken down into glucose, leading to a sharp rise in blood sugar levels. This spike triggers increased insulin release, which can stimulate androgen activity and promote excess sebum production within the sebaceous glands. Elevated IGF-1 levels may also accelerate follicular keratinization, a process where dead skin cells accumulate and contribute to clogged pores. Together, these changes create an environment where comedones such as blackheads and whiteheads are more likely to form, and where inflammation can develop more easily.
Beyond direct hormonal effects, dietary patterns associated with high glycemic intake may indirectly affect the skin barrier and inflammatory pathways. Diets rich in processed carbohydrates often lack essential nutrients that support skin repair and resilience, potentially weakening the skin’s ability to regulate oil production and maintain balanced cell turnover. In individuals already prone to acne due to genetic factors or hormonal fluctuations, this combination of increased sebum, disrupted keratinization, and impaired barrier function may increase the frequency or severity of breakouts. Environmental and lifestyle factors, including stress and inconsistent skincare habits, can further amplify these effects, making it difficult to isolate diet as the sole contributing factor.
While research exploring the relationship between high glycemic foods and acne continues to evolve, some evidence suggests that adopting a lower glycemic diet may help reduce acne severity in certain individuals. This approach typically emphasizes whole grains, legumes, vegetables, and proteins that produce a slower, more stable rise in blood sugar. However, dietary changes alone are rarely sufficient as a complete acne treatment. Evidence-based topical therapies remain central to managing clogged pores and inflammation. Ingredients such as salicylic acid are commonly used to penetrate pores and dissolve excess oil and debris, while retinoids help normalize skin cell turnover and reduce the formation of comedones. Benzoyl peroxide may help target acne-causing bacteria and reduce inflammatory lesions, and niacinamide is often recommended for its calming and oil-regulating properties.
For individuals with persistent or moderate to severe acne, professional dermatological care may be necessary. Dermatologists may recommend prescription-strength retinoids, oral medications that influence hormonal pathways, or in-office procedures designed to reduce inflammation and improve skin texture. These interventions are typically tailored to the individual’s skin type, acne severity, and underlying contributing factors, which may include diet, hormones, and genetics.
It is important to approach the connection between high glycemic foods and acne with realistic expectations. While dietary adjustments may support overall skin health and potentially reduce certain triggers, they are unlikely to produce immediate or universal results. Acne is a multifactorial condition, and effective management usually requires a combination of consistent skincare, lifestyle awareness, and, when needed, medical guidance. Individuals experiencing ongoing or severe acne are encouraged to consult a qualified healthcare professional to develop a personalized and evidence-based treatment plan.