Video 1
Video 2
Video 3
The skin barrier plays a central role in maintaining overall skin health, and its disruption is increasingly recognized as a contributing factor in acne development. The outermost layer of the skin, known as the stratum corneum, acts as a protective barrier that regulates water loss and shields against environmental irritants, bacteria, and allergens. This barrier is composed of tightly packed skin cells and lipids such as ceramides, cholesterol, and fatty acids. When intact, it helps maintain balanced hydration and supports normal skin function. However, when the barrier becomes damaged, it can trigger a cascade of changes that may contribute to acne formation.
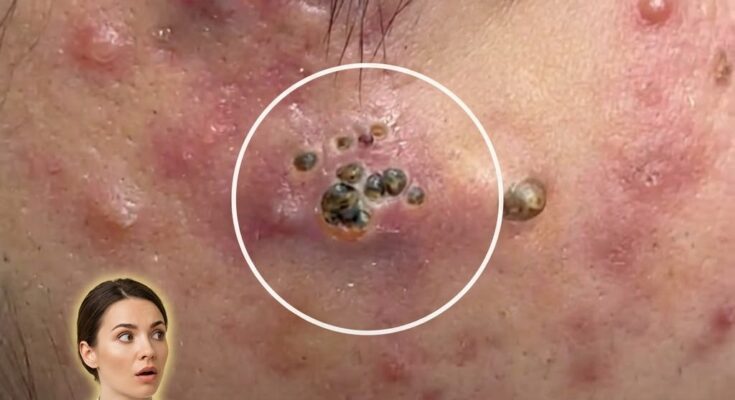
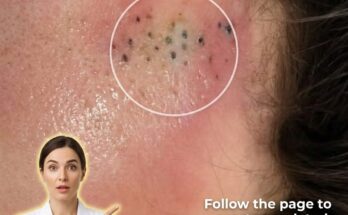
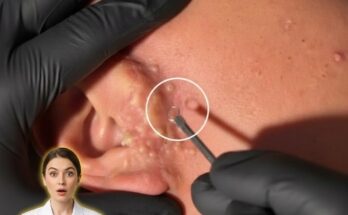
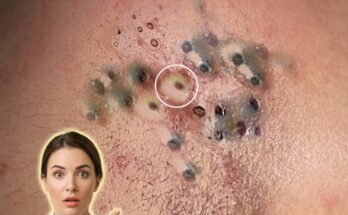
Barrier disruption often leads to increased transepidermal water loss, causing the skin to become dehydrated and more vulnerable to irritation. In response, the skin may attempt to compensate by producing more sebum. Excess sebum, combined with impaired shedding of dead skin cells, can contribute to clogged pores and the formation of comedones such as blackheads and whiteheads. Additionally, a weakened barrier may allow greater penetration of irritants and acne-causing bacteria, which can promote inflammation and lead to more noticeable breakouts.
Several factors can contribute to skin barrier damage. Overuse of harsh cleansers, excessive exfoliation, and frequent use of strong active ingredients like high-concentration acids or retinoids can disrupt the lipid matrix that holds the barrier together. Environmental stressors such as pollution, UV exposure, and low humidity may also weaken the barrier over time. In some individuals, genetic predisposition or underlying skin conditions can make the barrier more susceptible to damage. Hormonal fluctuations may further influence sebum production, compounding the effects of an already compromised barrier.
Addressing acne in the context of barrier damage often requires a balanced approach that focuses on both treating breakouts and restoring barrier function. Gentle cleansing with non-stripping formulations is commonly recommended to avoid further irritation. Ingredients such as ceramides, hyaluronic acid, and niacinamide may help support barrier repair by improving hydration and reinforcing the skin’s natural defenses. At the same time, acne-targeting ingredients like salicylic acid and benzoyl peroxide can still be used, but they are often best introduced gradually to minimize additional barrier disruption. Retinoids may also play a role by normalizing cell turnover, although careful use is important to prevent irritation.
In more persistent or severe cases, dermatological treatments may be considered. Professionals may recommend tailored topical therapies, barrier-repair moisturizers, or adjustments to existing skincare routines to reduce inflammation and improve skin resilience. The goal is often to create an environment where the skin can function more normally, reducing both acne formation and sensitivity.
It is important to recognize that repairing the skin barrier and improving acne does not happen immediately. The process typically requires consistent, gentle care over time. Overly aggressive treatments can prolong irritation and worsen both barrier damage and breakouts. Individuals experiencing ongoing or severe acne are encouraged to seek guidance from a qualified dermatologist, as personalized care can help address both the underlying causes and the visible symptoms more effectively.