Video 1
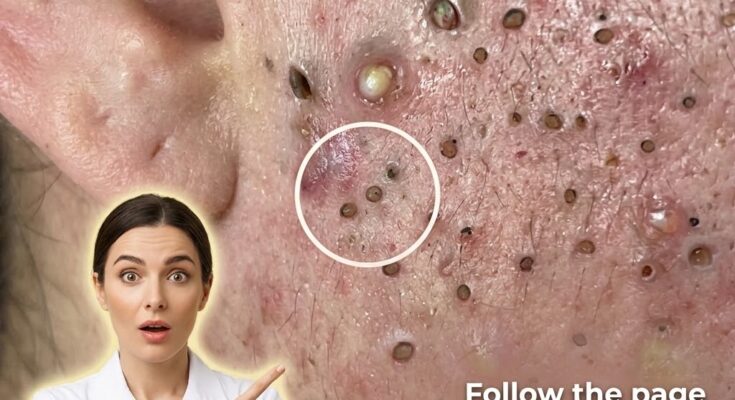
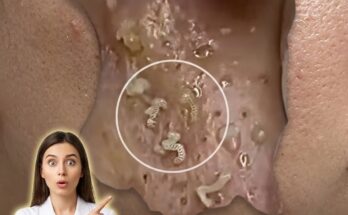
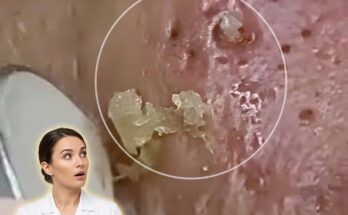
Acne-prone skin is strongly influenced by biological processes that regulate how the skin produces oil, sheds dead cells, and responds to inflammation. At the center of this process are the sebaceous glands, which produce sebum to maintain skin hydration. In individuals with a genetic predisposition to acne, these glands may be more active or more sensitive to hormonal signals, particularly androgens. This can lead to increased oil production, which mixes with dead skin cells inside the pore, contributing to follicular keratinization and the formation of clogged pores, including blackheads and whiteheads. When these clogged pores create an environment that supports bacterial growth, inflammation may follow, resulting in visible acne lesions.
Genetic factors also influence how efficiently the skin renews itself. Some individuals inherit a tendency toward slower or irregular shedding of skin cells, which increases the likelihood of comedone formation. In addition, variations in genes related to inflammation can affect how the immune system reacts to clogged pores. This helps explain why some people develop more inflamed acne, while others primarily experience non-inflammatory forms such as blackheads. Skin barrier function, which plays a role in protecting against irritation and maintaining hydration, may also be genetically influenced. A weaker barrier can make the skin more reactive to environmental triggers and skincare products, further complicating acne management.
While genetics set the baseline, other factors such as hormones, climate, and skincare habits can interact with this predisposition. For example, individuals who are genetically prone to oily skin may notice increased breakouts in humid environments or during periods of hormonal fluctuation. The use of overly harsh skincare products can disrupt the skin barrier, potentially worsening inflammation and triggering compensatory oil production. Conversely, consistent use of gentle, non-comedogenic products may help reduce the frequency of clogged pores, even in those with a strong genetic tendency toward acne.
Management of genetically influenced acne typically focuses on controlling the underlying processes rather than attempting to change the genetic predisposition itself. Ingredients such as retinoids are commonly used to normalize skin cell turnover and reduce the formation of comedones. Salicylic acid may help by penetrating into the pores and dissolving excess oil and debris, while benzoyl peroxide is often recommended for its antibacterial and anti-inflammatory properties. Niacinamide may also support skin barrier function and help regulate oil production, making it a useful addition for individuals with sensitive, acne-prone skin.
In cases where over-the-counter treatments are not sufficient, dermatological options such as prescription retinoids, hormonal therapies, or professional procedures may be considered. These approaches aim to address specific pathways involved in acne development, including sebum production and inflammation. However, responses to treatment can vary based on individual genetic differences, which is why personalized care is often important.
Although genetic factors cannot be changed, understanding their role can help set realistic expectations. Acne-prone skin may require ongoing management rather than a one-time solution. Consistent skincare routines, careful product selection, and professional guidance when needed can help minimize breakouts and support overall skin health over time.