Video 1
Video 2
Video 3
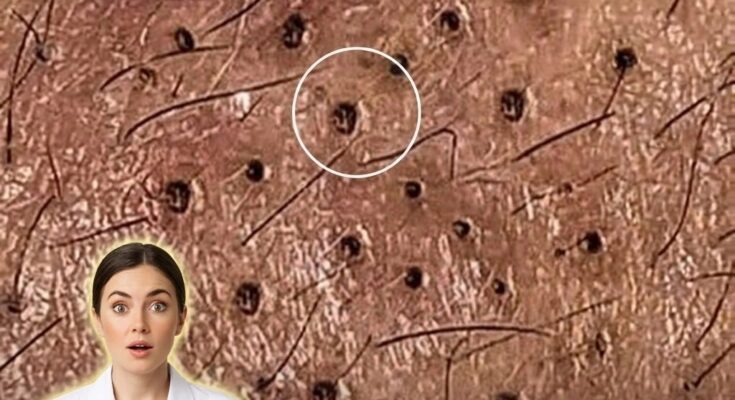
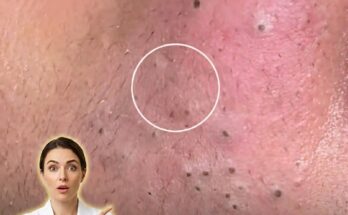
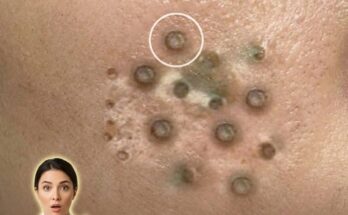
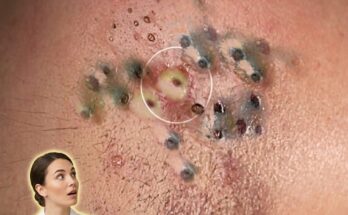
Inflammatory acne begins at the level of the hair follicle, where excess sebum production and abnormal shedding of skin cells combine to form a clogged pore, also known as a microcomedone. Within this enclosed environment, the buildup of oil and cellular debris creates conditions that allow Cutibacterium acnes to proliferate. As these bacteria interact with sebum, they can trigger an immune response in the surrounding skin. This response leads to the release of inflammatory mediators, causing redness, swelling, and tenderness that characterize early inflammatory lesions such as papules and pustules.
In the early stages, inflammation may not always be immediately visible on the surface. Subtle signs can include mild redness, sensitivity, or small raised bumps that develop from previously non-inflamed comedones like blackheads and whiteheads. The transition from non-inflammatory to inflammatory acne reflects a shift in the skin’s immune activity, where the follicle wall may become compromised, allowing inflammatory substances to spread into nearby tissue. This process contributes to the progression from simple pore blockage to more noticeable and sometimes painful lesions.
Several factors can influence how quickly and severely this inflammatory phase develops. Hormonal fluctuations, particularly androgens, can increase sebum production and make pores more prone to clogging. Skincare habits also play a role, as heavy or comedogenic products may contribute to congestion, while overly harsh cleansing or excessive use of active treatments can disrupt the skin barrier and exacerbate irritation. Environmental conditions such as heat and humidity may increase oil production and sweat, further affecting pore behavior. Genetic predisposition can also influence how reactive the immune system is to bacterial presence within the follicle.
Early management of inflammatory acne often focuses on reducing both pore congestion and bacterial activity while supporting the skin barrier. Ingredients such as salicylic acid are commonly used to penetrate pores and help dissolve excess oil and মৃত skin buildup. Benzoyl peroxide is frequently recommended for its ability to reduce acne-causing bacteria and calm inflammation. Topical retinoids may help normalize follicular keratinization, preventing the formation of new clogged pores and supporting long-term skin renewal. Niacinamide is also often included in skincare routines for its potential to soothe inflammation and regulate oil production.
Gentle skincare practices are important during this stage to avoid worsening inflammation. Using non-comedogenic moisturizers can help maintain barrier function, while daily sunscreen use supports overall skin health and reduces the risk of post-inflammatory discoloration. In cases where early inflammatory acne persists or worsens, dermatological treatments such as prescription retinoids, topical or oral antibiotics, or other targeted therapies may be considered under professional guidance.
The early stages of inflammatory acne are often manageable with consistent and appropriate care, but improvement typically takes time. Sudden or aggressive treatment approaches can sometimes irritate the skin and delay recovery. A gradual, balanced routine that addresses both clogged pores and inflammation is generally more effective. For individuals experiencing frequent or severe breakouts, consulting a qualified dermatologist can help ensure an accurate diagnosis and a tailored treatment plan that aligns with the skin’s specific needs.