Many people try to balance work and health by focusing only on daily habits.
While daily routines are important, they are only part of the bigger picture.
A healthy and productive life also benefits from a clear monthly flow.
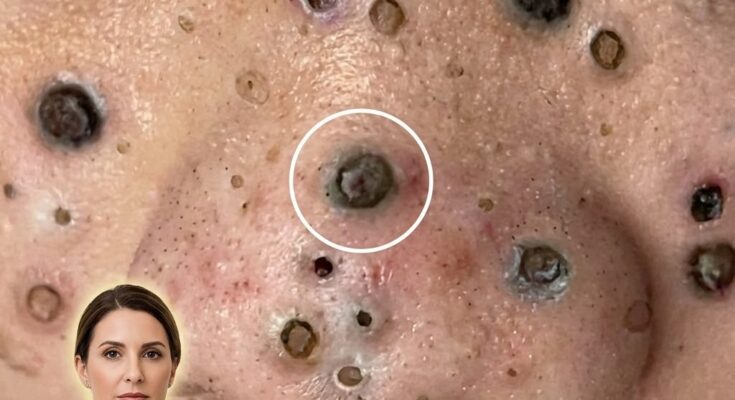
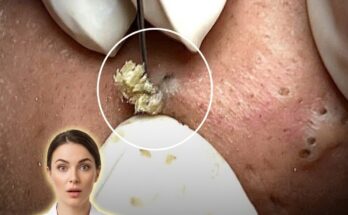
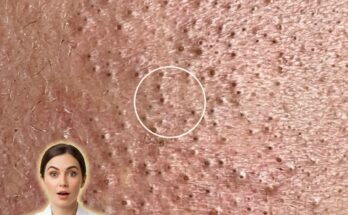
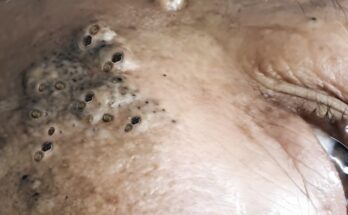
Insulin signaling plays an important role in several metabolic processes within the body, and growing research suggests it may also influence the biological pathways involved in acne development. Insulin is a hormone that regulates how cells absorb and use glucose for energy, but it also interacts with other hormonal systems that affect the skin. When insulin levels rise, particularly after consuming high-glycemic foods, the hormone can stimulate signaling pathways that increase the activity of insulin-like growth factor 1 (IGF-1). This compound may promote the proliferation of keratinocytes within hair follicles and stimulate sebaceous glands to produce more sebum. The combination of excess oil and increased shedding of skin cells inside the pore can contribute to follicular blockage, which is a central event in the formation of comedones such as blackheads and whiteheads.
Increased insulin and IGF-1 activity may also influence androgen signaling. Androgens are hormones that naturally stimulate sebaceous gland activity, and elevated androgen sensitivity within the skin can increase sebum production. When sebaceous glands produce more oil than the follicle can effectively drain, the environment within the pore becomes more prone to congestion. This process may allow dead skin cells and oil to accumulate, forming the microcomedone that precedes visible acne lesions. Over time, these clogged pores can evolve into inflammatory acne if bacteria within the follicle trigger immune responses.
Dietary patterns may play a role in how strongly insulin signaling affects the skin. Foods that cause rapid spikes in blood glucose, often described as high glycemic index foods, can lead to increased insulin release. Repeated elevations in insulin may amplify IGF-1 signaling and reduce levels of certain proteins that normally regulate androgen activity. While diet alone does not cause acne in every individual, research suggests that dietary patterns characterized by frequent high-glycemic foods may contribute to oil production and pore congestion in people who are already acne-prone. Genetic factors, hormonal fluctuations, and individual metabolic responses all influence how strongly insulin pathways affect the skin.
Insulin signaling may also interact with inflammation, which is a key component of acne lesions. Elevated insulin and IGF-1 activity can influence inflammatory mediators and cellular growth pathways within the skin. In acne-prone individuals, this environment may increase the likelihood that clogged pores progress into inflamed papules or pustules. In addition, insulin-related pathways can influence the rate of skin cell turnover inside the follicle, which may contribute to the buildup of keratin and debris that obstructs pores.
Managing acne influenced by metabolic and hormonal pathways often involves a combination of skincare and broader lifestyle considerations. Topical ingredients that help regulate follicular turnover and reduce pore congestion are commonly used in dermatology-based skincare routines. Retinoids are frequently recommended because they normalize the shedding of skin cells inside the pore and help prevent the formation of new comedones. Salicylic acid is another widely used ingredient that penetrates oil within the pore and helps loosen accumulated debris. Benzoyl peroxide may help reduce acne-causing bacteria and limit inflammation, while niacinamide is often included in formulations designed to support the skin barrier and reduce redness associated with breakouts.
For individuals whose acne appears strongly influenced by hormonal factors, dermatologists may consider additional treatment approaches. Certain prescription medications can help regulate androgen signaling or improve skin cell turnover. Professional guidance may also include evaluating overall health factors that affect insulin sensitivity, particularly in cases where acne is persistent or accompanied by other metabolic symptoms. These assessments help ensure that treatment plans address both the skin and the underlying biological pathways contributing to breakouts.
Although insulin signaling appears to play a meaningful role in acne biology for some individuals, acne is a multifactorial condition involving hormones, genetics, microbial activity, inflammation, and skincare habits. Improvements in acne typically require consistent treatment over time, and results may vary depending on individual physiology. Evidence-based skincare routines and guidance from qualified dermatology professionals can help individuals develop safe and realistic strategies for managing acne while protecting overall skin health.