Discovering the World of Arthropods
When we think about the wonders of nature, our minds often drift to majestic mountains, serene lakes, or vibrant flower gardens.
Yet, nestled within these landscapes is a hidden realm that is both fascinating and surprisingly diverse: the world of arthropods.
These remarkable creatures, which include insects, spiders, crabs, and more, make up the largest group of animals on our planet.
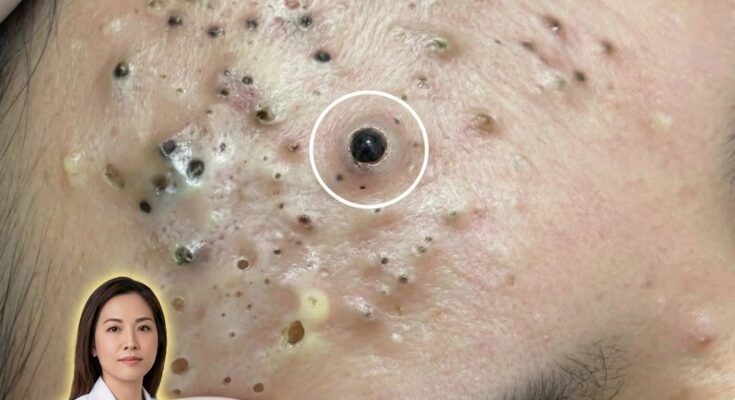
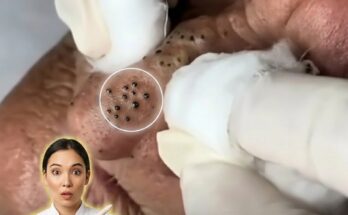
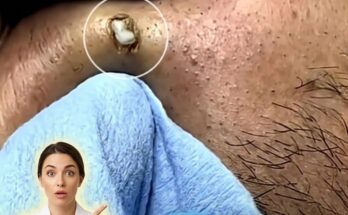
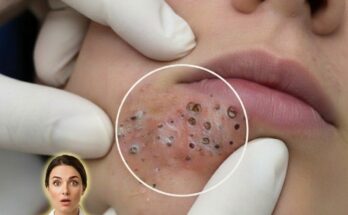
Stress is increasingly recognized as a factor that can influence several biological processes involved in acne development, including sebum production. Sebum is an oily substance produced by sebaceous glands located within hair follicles. Under normal conditions, sebum helps lubricate the skin and maintain barrier function. However, when sebum production becomes excessive, it can combine with dead skin cells inside pores and contribute to the formation of clogged pores, blackheads, and whiteheads. Hormonal signals play a major role in regulating sebaceous gland activity, and stress-related hormones may indirectly alter this regulation in ways that promote oilier skin.
When the body experiences psychological or physical stress, the hypothalamic–pituitary–adrenal axis becomes activated. This process leads to the release of stress hormones such as cortisol and corticotropin-releasing hormone. Research suggests that these hormones can influence sebaceous glands by increasing lipid synthesis within the cells that produce sebum. In addition, corticotropin-releasing hormone receptors have been identified directly within sebaceous glands, indicating that the skin may respond locally to stress signals. As a result, individuals under prolonged or intense stress may notice increased oiliness, which can contribute to the development of comedones and other acne lesions.
Stress may also influence other biological mechanisms involved in clogged pore formation. Elevated cortisol levels can affect the skin barrier, potentially increasing transepidermal water loss and making the skin more susceptible to irritation. In response, the skin may increase sebum production as a compensatory mechanism. Stress can also influence inflammatory signaling in the skin, which may worsen the progression of acne lesions once pores become congested. These combined effects help explain why periods of emotional stress are commonly associated with acne flare-ups in both adolescents and adults.
Lifestyle behaviors that often accompany stress may further contribute to breakouts. Irregular sleep patterns, changes in diet, increased consumption of high-glycemic foods, and inconsistent skincare routines can all affect skin physiology. Additionally, individuals experiencing stress may be more likely to touch or pick at their skin, which can aggravate clogged pores and increase the risk of inflammation or post-inflammatory marks. While stress itself may not be the sole cause of acne, it can interact with existing factors such as hormonal fluctuations, oily skin, and genetic predisposition.
Evidence-based skincare approaches aim to regulate pore function and reduce the conditions that allow clogged pores to form. Ingredients such as salicylic acid are commonly used to penetrate oily pores and help dissolve the mixture of sebum and dead skin cells. Topical retinoids are frequently recommended in dermatology because they help normalize skin cell turnover and reduce follicular keratinization, which is a key step in comedone formation. Benzoyl peroxide may also be used to reduce acne-causing bacteria and inflammation when breakouts become more active. Niacinamide is another ingredient that may help regulate oil production while supporting the skin barrier.
For individuals who experience stress-related acne flare-ups, maintaining a consistent skincare routine may help reduce the impact of hormonal fluctuations on the skin. Gentle cleansing, regular use of non-comedogenic moisturizers, and gradual introduction of active ingredients can support balanced skin function. Stress-management practices such as adequate sleep, regular exercise, and mindfulness techniques may also support overall hormonal balance, which can indirectly benefit the skin.
Although stress management and skincare can help reduce contributing factors, persistent or severe acne may require evaluation by a dermatologist. Prescription topical retinoids, hormonal therapies, or other targeted treatments may be recommended depending on the type and severity of acne. Because acne development involves multiple biological pathways, improvements often occur gradually rather than immediately. A consistent, evidence-based approach remains one of the most reliable ways to manage acne while supporting long-term skin health.