Video 1
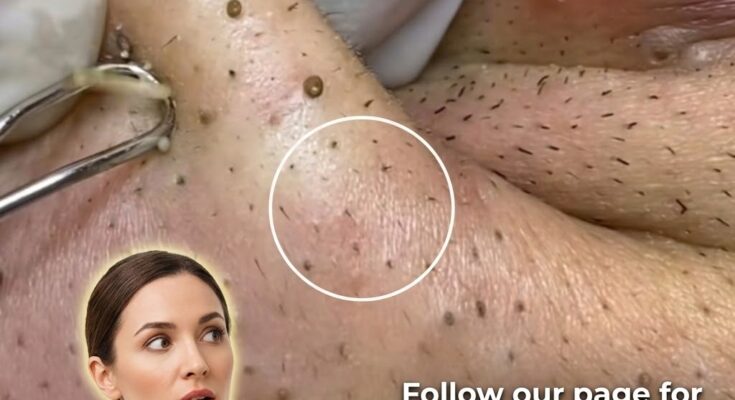
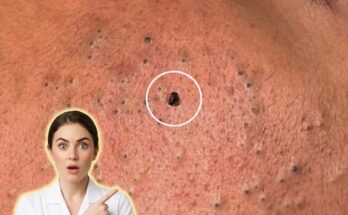
Clogged pores represent one of the earliest and most fundamental steps in acne development, and the skin’s defensive response to this process plays a central role in whether a minor blockage remains non-inflammatory or progresses into visible breakouts. At the microscopic level, pores are connected to sebaceous glands that produce sebum, an oily substance that helps maintain hydration and barrier integrity. When excess sebum combines with dead skin cells that are not shed efficiently, a plug forms within the follicle, a process known as follicular keratinization. This creates an environment where oxygen levels decrease, altering the balance of skin microbes and setting the stage for an immune response .
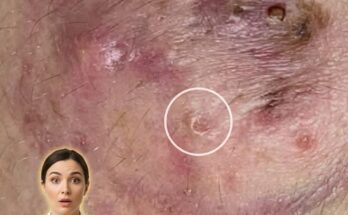
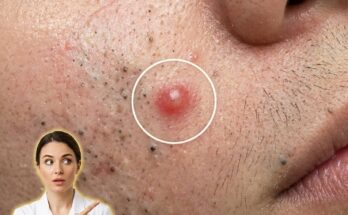
As the pore becomes increasingly obstructed, the skin begins to recognize this buildup as a potential threat. Cells within the follicle release signaling molecules that activate the innate immune system. This response is not always aggressive at first, which is why some clogged pores remain as blackheads or whiteheads without redness or pain. However, if the blockage persists, certain bacteria such as Cutibacterium acnes may proliferate within the low-oxygen environment. The immune system reacts by sending inflammatory mediators to the area, increasing blood flow and triggering the redness, swelling, and tenderness commonly associated with inflamed acne lesions.
Several internal and external factors can influence how strongly the skin reacts to clogged pores. Hormonal fluctuations, particularly increases in androgens, may stimulate higher sebum production, making blockages more likely. Skincare habits also play a role, as overly harsh cleansing or excessive use of active treatments can disrupt the skin barrier, potentially amplifying inflammatory responses. Environmental factors such as humidity, pollution, and friction from clothing or masks may further contribute to pore congestion and irritation. Genetic predisposition can also affect how reactive an individual’s immune system is to follicular blockage, which partly explains why acne severity varies widely between individuals.
Management strategies often focus on both preventing pore blockage and moderating the skin’s defensive response. Ingredients such as salicylic acid are commonly used because they are oil-soluble and can penetrate into pores to help dissolve excess sebum and dead skin buildup. Retinoids are frequently recommended as they normalize cell turnover and reduce the formation of comedones over time. Benzoyl peroxide may help reduce bacterial load within the follicle, indirectly decreasing inflammatory signaling. Niacinamide is often included in formulations for its potential to support the skin barrier and modulate inflammation, which may help calm reactive skin.
Professional treatments may be considered when over-the-counter approaches are insufficient. Dermatologists may recommend prescription-strength retinoids, combination therapies, or procedures such as chemical peels or extractions, depending on the type and severity of acne. These approaches aim to address both the physical blockage within pores and the immune processes that drive inflammation.
It is important to recognize that the skin’s defensive reaction is not inherently harmful; it is a protective mechanism designed to maintain balance and respond to perceived threats. However, when this response becomes exaggerated or prolonged, it contributes to the visible and sometimes persistent nature of acne. Improvements typically occur gradually, as treatments work to regulate both pore function and inflammatory activity over time. Consistent, gentle skincare and appropriate use of active ingredients are often key, and individuals with persistent or severe symptoms may benefit from consultation with a qualified dermatology professional.