Career exploration is an important step in every student’s journey.
Choosing a future path can feel overwhelming, especially with so many professions and opportunities available today.
However, exploring careers early helps students understand their interests, develop useful skills, and make more confident decisions about education and work.
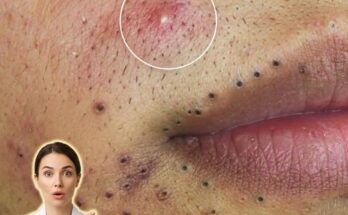
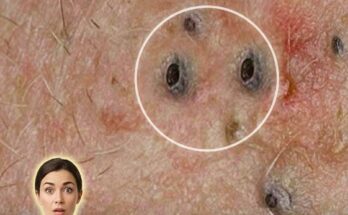
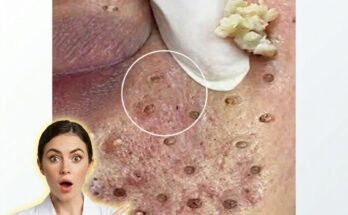
Microcomedones represent the earliest microscopic stage in the development of many acne lesions. They form within the pilosebaceous unit, a structure consisting of a hair follicle, sebaceous gland, and the tiny canal that allows sebum to reach the skin surface. Under normal conditions, skin cells lining the follicle shed gradually and are carried out of the pore with sebum. In acne-prone skin, however, this process becomes disrupted. Skin cells may begin to accumulate and stick together within the follicle, mixing with sebum to create a small plug beneath the skin surface. This early blockage, invisible to the eye, is known as a microcomedone and is considered the starting point for both blackheads and whiteheads.
The biological process responsible for this buildup is often described as abnormal follicular keratinization. Keratinocytes, the cells that form the outer layer of the skin, may shed more rapidly while also becoming more adhesive. Instead of dispersing individually, these cells cluster together and combine with sebum produced by nearby sebaceous glands. The resulting mixture gradually accumulates in the follicular canal. Because the plug forms deep within the pore at this stage, the skin surface may still appear relatively normal even though the earliest acne lesion has already begun developing.
Sebum production plays an important role in this process. Sebaceous glands naturally produce oil to help lubricate the skin and maintain barrier function. In individuals with oily skin or hormonally stimulated sebaceous glands, higher levels of sebum can increase the likelihood that follicular debris becomes trapped. Hormones known as androgens are particularly influential because they stimulate sebaceous gland activity. During adolescence, hormonal fluctuations, stress responses, or certain medical conditions may increase androgen signaling, which can contribute to excess oil production and support the formation of microcomedones.
Genetic factors may also influence how easily microcomedones form. Some individuals appear to inherit sebaceous glands that produce more oil or follicles that are more prone to keratin buildup. These inherited tendencies can help explain why acne sometimes runs in families and why certain people develop persistent clogged pores despite maintaining consistent skincare habits.
Environmental influences and skincare practices may further affect the development of these early lesions. Heavy occlusive products, inadequate cleansing after sweating, or repeated friction against the skin may contribute to conditions that allow keratin and oil to accumulate in pores. At the same time, excessive cleansing or harsh exfoliation can disrupt the skin barrier, which may trigger compensatory oil production and irritation that worsens follicular blockage. Maintaining balanced skincare practices is often considered an important factor in supporting normal pore function.
As a microcomedone grows, it may eventually become visible as either a closed comedone or an open comedone. Closed comedones, often called whiteheads, occur when the pore opening remains covered by a thin layer of skin. Open comedones, commonly known as blackheads, form when the pore opening enlarges and the accumulated material becomes exposed to air, allowing oxidation to darken the surface of the plug. In some cases, bacteria associated with acne, particularly Cutibacterium acnes, may multiply within the clogged follicle and trigger inflammatory lesions such as papules or pustules.
Because microcomedones form beneath the skin before visible acne appears, many acne treatments focus on preventing this early blockage. Topical retinoids are widely used in dermatology because they help normalize the shedding of skin cells within the follicle, which may reduce the formation of new comedones over time. Ingredients such as salicylic acid are also commonly included in acne skincare routines because they are oil-soluble and can penetrate into pores to help loosen accumulated debris. Other supportive ingredients, including niacinamide and gentle exfoliating acids, may help regulate oil production and improve overall skin barrier balance.
Professional dermatology treatments may be recommended for individuals with persistent comedonal acne. Dermatologists sometimes prescribe stronger retinoids, combination therapies containing benzoyl peroxide, or procedures such as chemical peels that help promote controlled exfoliation of the follicular lining. These approaches are designed to reduce the number of new microcomedones forming beneath the surface while addressing existing clogged pores.
It is important to recognize that the formation of microcomedones is a continuous biological process in acne-prone skin. Even when visible lesions improve, new microscopic blockages may still be developing below the surface. For this reason, acne treatments often require consistent use over several weeks or months before noticeable improvements occur. Individuals experiencing persistent or severe acne may benefit from consulting a qualified dermatologist who can evaluate underlying factors and recommend an appropriate long-term treatment strategy.