Video 1
Video 2
Video 3
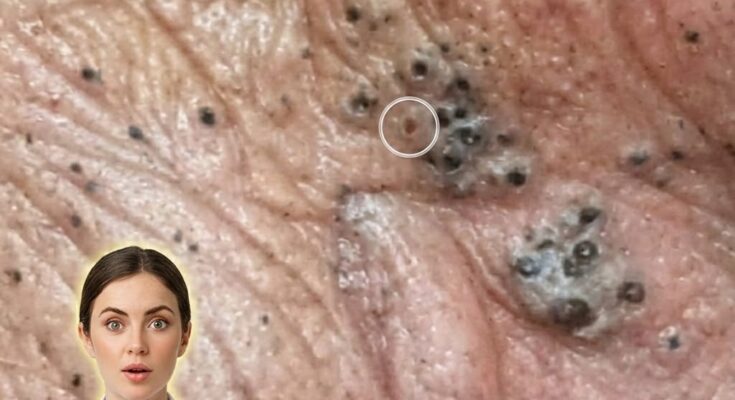
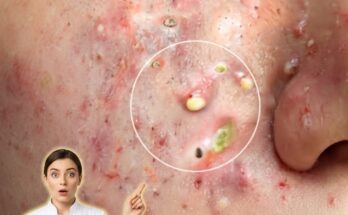
Microbial imbalance on the skin, often referred to as disruption of the skin microbiome, plays a significant role in the development and persistence of acne breakouts. The skin naturally hosts a diverse community of microorganisms, including bacteria such as Cutibacterium acnes, which typically exist in balance with other microbes and the skin’s immune system. Under stable conditions, this ecosystem helps maintain skin health by supporting barrier function and preventing colonization by harmful organisms. However, when this balance is disrupted, certain microbial populations may become dominant, contributing to inflammation, clogged pores, and the formation of comedones such as blackheads and whiteheads.
One of the key mechanisms behind microbial imbalance involves the interaction between excess sebum production and follicular keratinization. Increased oil production, often influenced by hormonal fluctuations, creates an environment where Cutibacterium acnes can thrive. As dead skin cells accumulate and mix with sebum inside the pores, blockages form, limiting oxygen availability. This low-oxygen environment favors the proliferation of specific strains of C. acnes that may trigger inflammatory responses. At the same time, beneficial microbes that help regulate skin immunity may decline, further weakening the skin’s natural defenses and allowing inflammation to escalate.
External and lifestyle factors can also contribute to microbial imbalance. Harsh cleansing routines, overuse of exfoliating acids, or frequent application of strong acne treatments may disrupt the skin barrier, altering the microbiome. Environmental stressors such as pollution and humidity can influence microbial diversity, while certain cosmetic products may either support or hinder a balanced skin environment depending on their formulation. Genetic predisposition can also affect how an individual’s immune system responds to microbial shifts, making some people more prone to inflammatory acne.
Addressing microbial imbalance in acne-prone skin typically involves approaches that aim to restore balance rather than eliminate all bacteria. Ingredients such as benzoyl peroxide are commonly used to reduce bacterial overgrowth, while salicylic acid helps clear clogged pores by dissolving oil and debris within the follicle. Retinoids are often recommended to normalize skin cell turnover, reducing the formation of comedones and indirectly influencing the microbial environment. Niacinamide may help support the skin barrier and reduce inflammation, creating conditions that are less favorable for imbalance. In some cases, dermatological treatments, including topical or oral antibiotics, may be considered, although their use is generally monitored to minimize disruption of beneficial microbes.
Maintaining a consistent and balanced skincare routine is an important part of managing microbial health. Gentle cleansing, appropriate moisturization, and gradual introduction of active ingredients may help support the skin barrier while reducing the risk of irritation-driven imbalance. It is also important to recognize that changes in the microbiome do not resolve immediately, and improvements in acne may take time as the skin gradually stabilizes.
Overall, microbial imbalance is one of several interconnected factors that contribute to acne development. While skincare ingredients and treatments can help manage breakouts, outcomes vary depending on individual skin characteristics and underlying causes. Persistent or severe acne may benefit from evaluation by a qualified dermatologist, who can provide tailored guidance based on the specific needs of the skin.