Video 1
Video 2
Video 3
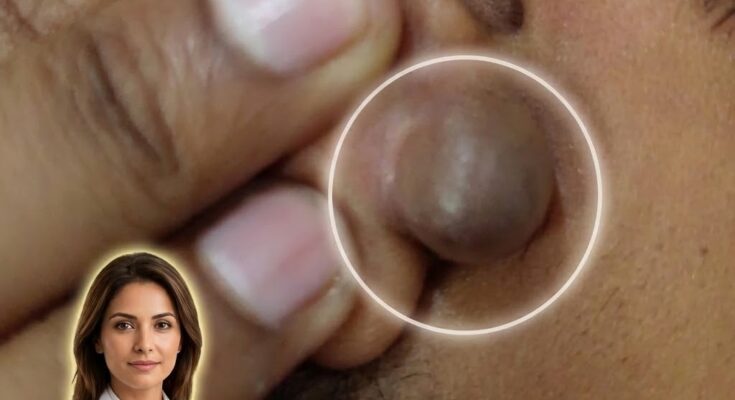
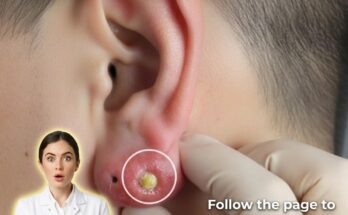
Hormonal fluctuations during the menstrual cycle can influence several biological processes in the skin that are closely linked to acne development. Acne forms when hair follicles become clogged with excess sebum and dead skin cells, a process known as follicular keratinization. Hormones regulate many aspects of this process. Androgens, which are present in both males and females, stimulate sebaceous glands to produce oil. When androgen activity increases relative to other hormones, the sebaceous glands may produce more sebum, creating an environment where clogged pores, blackheads, whiteheads, and inflamed acne lesions can more easily develop.
Throughout the menstrual cycle, levels of estrogen, progesterone, and androgens shift in a predictable pattern. In the first half of the cycle, often called the follicular phase, estrogen levels gradually rise. Estrogen is generally associated with stabilizing effects on the skin and may help limit excessive oil production. During this time, some individuals notice relatively calmer skin. After ovulation, progesterone levels increase during the luteal phase. Progesterone can indirectly influence sebaceous gland activity and may also affect the way skin cells shed within the follicle, which can contribute to pore congestion.
In the days leading up to menstruation, estrogen and progesterone levels both decline. During this period, the relative influence of androgens may become more noticeable. This hormonal shift can stimulate increased sebum production and may promote the formation of comedones within pores. As pores become clogged with oil and keratinized cells, bacteria that naturally live on the skin can trigger inflammation. This is one reason why many people experience more noticeable breakouts along the jawline, chin, and lower cheeks shortly before their menstrual cycle begins.
Several additional factors may influence how strongly the menstrual cycle affects acne severity. Genetics can play a role in determining how responsive sebaceous glands are to hormones. Individuals with naturally oily skin or larger pores may be more prone to experiencing hormonal breakouts. Stress may also interact with hormonal activity, as elevated stress hormones can further stimulate oil production and inflammation. Skincare habits can influence this process as well, particularly when products are overly occlusive or when harsh cleansing disrupts the skin barrier and triggers compensatory oil production.
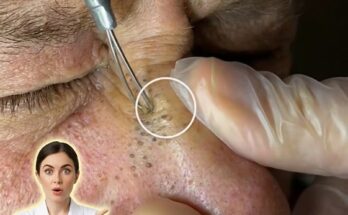
Evidence-informed skincare strategies are often used to help manage hormonally influenced acne. Ingredients that regulate pore congestion are commonly recommended. Topical retinoids may help normalize follicular keratinization and reduce the formation of clogged pores. Salicylic acid is frequently used to penetrate oil within the follicle and assist with clearing blackheads and whiteheads. Benzoyl peroxide may help reduce acne-causing bacteria and inflammatory lesions. Niacinamide is sometimes included in skincare routines because it may support the skin barrier and help regulate oil production while calming visible redness.
For individuals with persistent or severe hormonal acne, dermatology professionals may recommend additional treatment approaches. Prescription retinoids, hormonal therapies such as certain oral contraceptives, or medications that reduce androgen activity are sometimes used when over-the-counter skincare is not sufficient. It is important to understand that hormonal acne management typically focuses on controlling the underlying processes rather than providing an immediate cure. Breakouts related to menstrual cycles may still occur periodically, but consistent treatment and supportive skincare routines can often help reduce their frequency and severity. Individuals experiencing ongoing or worsening acne are generally encouraged to consult a qualified healthcare professional to determine the most appropriate treatment plan.