Video 1
Video 2
Video 3
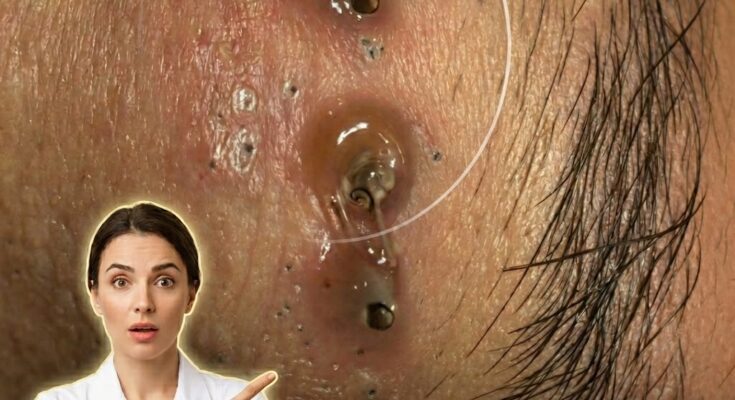
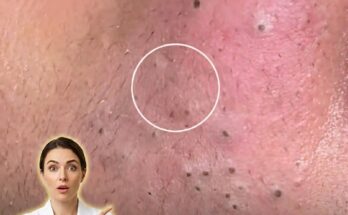
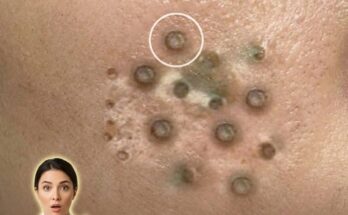
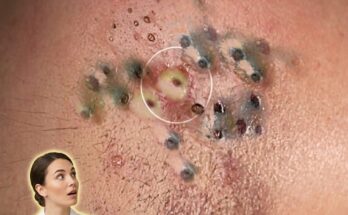
Acne develops through a combination of biological processes involving excess sebum production, abnormal shedding of dead skin cells, and the formation of clogged pores known as comedones. These blockages create an environment where bacteria can proliferate and trigger inflammation, leading to blackheads, whiteheads, and more inflamed lesions. While genetic predisposition plays a role in how active these processes are, lifestyle factors can significantly influence their intensity by affecting hormonal balance, skin barrier function, and oil production.
Diet is one of the most discussed lifestyle contributors to acne. High glycemic foods, which rapidly increase blood sugar levels, may stimulate insulin and insulin-like growth factor 1 (IGF-1), both of which can increase sebum production and promote follicular keratinization. This process can make pores more prone to clogging. Dairy consumption has also been associated in some individuals with increased acne activity, potentially due to hormonal components that may influence androgen signaling. These dietary patterns do not affect everyone equally, but they may contribute to breakouts in acne-prone skin.
Stress is another important factor that may worsen acne through hormonal pathways. Elevated stress levels can increase cortisol, which may indirectly stimulate oil glands and exacerbate inflammation in the skin. In addition, stress can impair skin barrier function, making the skin more reactive and slower to recover from existing lesions. Sleep quality is closely related, as inadequate sleep may disrupt hormonal regulation and immune responses, potentially prolonging acne healing and increasing susceptibility to new breakouts.
Skincare habits also play a significant role in either supporting or disrupting skin health. Over-cleansing, harsh exfoliation, or the use of irritating products can damage the skin barrier, leading to increased transepidermal water loss and compensatory oil production. On the other hand, inadequate cleansing may allow excess sebum, dead skin cells, and environmental debris to accumulate within pores, contributing to blackheads and whiteheads. The use of comedogenic products, including certain heavy oils or occlusive formulations, may further increase the likelihood of pore congestion in susceptible individuals.
Environmental and lifestyle exposures such as humidity, pollution, and frequent contact with occlusive materials can also influence acne development. High humidity may increase sweat and oil production, while airborne pollutants can settle on the skin and contribute to oxidative stress and inflammation. Mechanical factors, such as friction from masks, helmets, or tight clothing, can lead to a type of acne often referred to as acne mechanica, where repeated pressure and occlusion promote clogged pores and irritation.
Management of acne influenced by lifestyle factors typically involves a combination of consistent skincare and targeted treatments. Ingredients such as salicylic acid may help exfoliate inside the pore and reduce congestion, while retinoids are commonly used to normalize skin cell turnover and prevent comedone formation. Benzoyl peroxide may help reduce acne-causing bacteria and inflammation, and niacinamide is often included to support the skin barrier and regulate oil production. Adjustments in diet, stress management, and sleep hygiene may also contribute to overall skin improvement, although results can vary between individuals.
It is important to recognize that lifestyle modifications alone may not fully resolve acne, particularly in moderate to severe cases where underlying hormonal or genetic factors are significant. Improvements tend to occur gradually, and consistent habits are required to support long-term skin health. Individuals experiencing persistent or worsening acne are often advised to consult a qualified healthcare professional or dermatologist, who can recommend personalized treatment strategies and ensure that underlying conditions are appropriately addressed.