Video 1
Video 2
Video 3
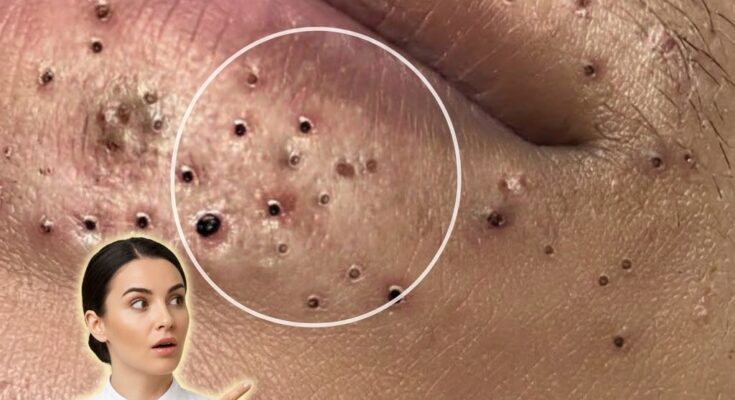
Cutibacterium acnes, a bacterium naturally present on human skin, plays a central role in how acne develops through its interaction with sebum, the oily substance produced by sebaceous glands. Sebum is composed of lipids such as triglycerides, wax esters, and squalene, and it helps maintain skin hydration and barrier function under normal conditions. However, when sebum production increases, particularly under the influence of androgens, it creates an environment within the hair follicle that supports the growth of Cutibacterium acnes. This bacterium thrives in low-oxygen, lipid-rich environments and uses enzymes called lipases to break down triglycerides in sebum into free fatty acids. These byproducts can irritate the follicular lining and contribute to inflammation, which is a key feature in acne development .
As Cutibacterium acnes metabolizes sebum, it also interacts with the immune system. The presence of bacterial components and inflammatory mediators can activate immune cells, leading to redness, swelling, and the formation of inflammatory lesions such as papules and pustules. At the same time, excess sebum can combine with dead skin cells in a process known as follicular keratinization, leading to clogged pores. These clogged pores may appear as blackheads or whiteheads, and they create a closed environment where bacterial activity can further intensify. This interaction between oil production, bacterial growth, and immune response explains why acne is not simply a hygiene issue but a complex biological process.
Several contributing factors can influence how strongly Cutibacterium acnes interacts with skin oil. Hormonal fluctuations, especially during puberty or periods of hormonal imbalance, can increase sebum production and make pores more prone to congestion. Skincare habits also play a role, as the use of heavy or occlusive products may trap oil and debris within pores, while over-cleansing or harsh exfoliation can disrupt the skin barrier and trigger compensatory oil production. Environmental factors such as humidity and pollution may further alter sebum composition, while genetic predisposition can affect both oil production levels and inflammatory sensitivity.
Managing this interaction often involves targeting multiple points in the acne pathway. Ingredients such as salicylic acid are commonly used because they are oil-soluble and can penetrate into pores to help dissolve excess sebum and debris. Retinoids are widely recommended for regulating cell turnover and reducing follicular clogging, which indirectly limits the environment in which Cutibacterium acnes thrives. Benzoyl peroxide is frequently used for its antibacterial properties, as it can reduce bacterial populations on the skin. Niacinamide may help regulate oil production and support the skin barrier while also providing anti-inflammatory benefits. In more persistent cases, dermatological treatments such as topical or oral medications may be considered to further control bacterial activity and inflammation.
It is important to recognize that Cutibacterium acnes is a normal part of the skin microbiome and not inherently harmful. Acne develops when there is an imbalance involving sebum production, pore blockage, and inflammation. Effective skincare focuses on restoring balance rather than completely eliminating bacteria or oil. Results from treatments may take several weeks to become noticeable, and overuse of aggressive products can worsen irritation. For individuals experiencing moderate to severe or persistent acne, consultation with a qualified dermatologist is recommended to develop a treatment plan tailored to their skin’s specific needs.