Video 1
Video 2
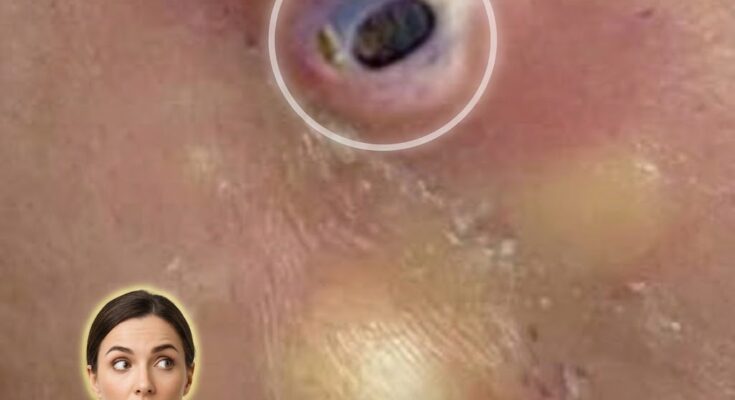
Whiteheads and blackheads are both forms of comedonal acne, meaning they originate from the same fundamental process within the skin’s hair follicles. The key mechanism begins with excess sebum production combined with abnormal shedding of dead skin cells, a process known as follicular keratinization. When these materials accumulate inside a pore, they form a plug called a comedone. Whether that comedone becomes a whitehead or a blackhead depends primarily on whether the pore remains closed or becomes exposed to air.
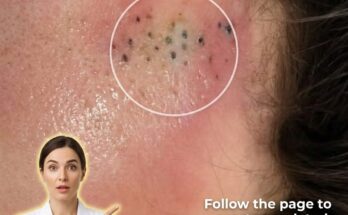
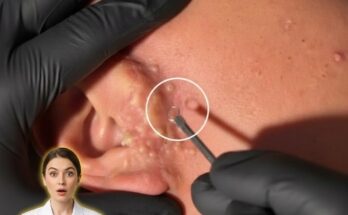
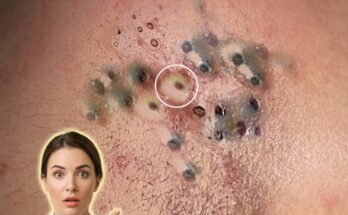
A whitehead, also known as a closed comedone, forms when the pore opening stays sealed. The trapped mixture of oil, dead skin cells, and cellular debris remains beneath the surface, creating a small, flesh-colored or white bump. Because the contents are not exposed to oxygen, there is no oxidation process, and the material inside retains its lighter appearance. In contrast, a blackhead, or open comedone, occurs when the pore opening widens. This allows the contents to be exposed to air, leading to oxidation of melanin and lipids within the plug, which gives the surface its characteristic dark color. This dark appearance is not due to dirt, as is commonly misunderstood, but rather a chemical reaction at the skin’s surface.
Several contributing factors influence whether someone develops more whiteheads or blackheads. Increased sebum production, often driven by hormonal fluctuations such as those occurring during puberty or periods of stress, can create an environment where pores are more easily clogged. Skin type also plays a role, with oily skin being more prone to both forms of comedones. External factors such as the use of comedogenic skincare or cosmetic products may further contribute by blocking pores. Environmental elements, including humidity and pollution, can also interact with the skin’s surface, potentially worsening pore congestion. Genetics may influence how efficiently the skin sheds dead cells and regulates oil production, which can predispose individuals to recurring comedonal acne.
Treatment approaches for whiteheads and blackheads often overlap because they target the same underlying processes. Ingredients that help normalize skin cell turnover, such as retinoids, are commonly recommended because they reduce the buildup of dead skin cells within the pore lining. Salicylic acid, a beta hydroxy acid, is frequently used due to its ability to penetrate into the pore and dissolve excess sebum and debris, making it particularly useful for blackheads. Benzoyl peroxide may be included in some routines, especially when inflammatory acne is also present, as it helps reduce acne-causing bacteria. Niacinamide is another ingredient that may support overall skin balance by helping regulate oil production and improving the skin barrier function. Consistent, gentle cleansing and avoiding overly harsh scrubbing are also important, as irritation can worsen keratinization and lead to more clogged pores.
Professional dermatological treatments may be considered when over-the-counter options are not sufficient. These can include chemical peels designed to exfoliate the skin more deeply, manual extraction performed under sterile conditions, or prescription-strength retinoids that provide more potent regulation of cell turnover. In some cases, dermatologists may tailor treatment based on whether closed or open comedones are more dominant, as whiteheads can sometimes be more resistant due to their closed structure.
While whiteheads and blackheads are biologically similar, their visible differences reflect how the pore behaves at the surface of the skin. Both are non-inflammatory forms of acne, but if left untreated, they may progress into inflamed lesions such as papules or pustules. Managing them effectively typically requires consistent skincare, patience, and realistic expectations, as improvements often occur gradually over weeks to months. For persistent or severe cases, consulting a qualified skincare professional or dermatologist is advisable to ensure an appropriate and safe treatment plan.