Video 1
Video 2
Video 3
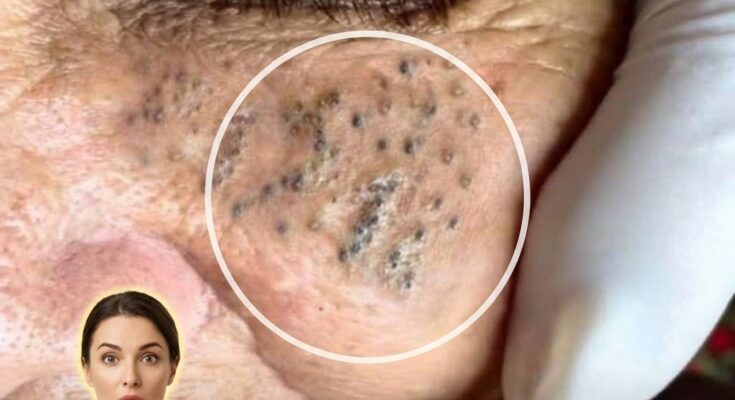
Acne management is not a one-time solution because the condition is driven by ongoing biological processes within the skin rather than a temporary imbalance. At the level of the pilosebaceous unit, acne develops through continuous interactions between sebum production, follicular keratinization, microbial activity, and inflammation. Even when visible lesions improve, these underlying mechanisms often remain active, meaning the skin retains a tendency to form new clogged pores and breakouts over time.
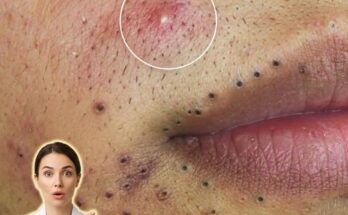
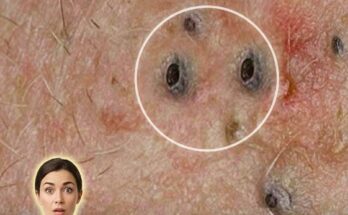
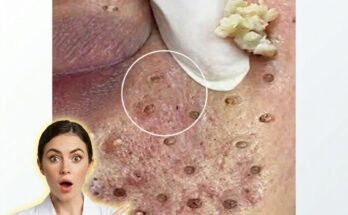
One of the main reasons acne persists or recurs is the influence of hormones. Androgens stimulate sebaceous glands to produce sebum, and this activity can fluctuate throughout life due to factors such as age, stress, and natural hormonal cycles. Because these signals are ongoing, oil production does not permanently “switch off” after treatment. This continuous sebum flow can combine with dead skin cells inside the follicle, leading to the repeated formation of microcomedones, which later develop into blackheads, whiteheads, or inflamed acne.
Skin cell turnover is another process that requires long-term regulation. In acne-prone individuals, keratinocytes within the follicle tend to shed irregularly, increasing the likelihood of blockage. Treatments such as retinoids are commonly used to normalize this process, but their effects depend on continued use. When treatment is stopped, the skin gradually returns to its baseline behavior, and the conditions that led to acne may reappear.
Inflammation also contributes to why acne cannot be considered a one-time issue. Even when the skin looks clear, low-level inflammation may persist beneath the surface. This subclinical inflammation can make the skin more reactive and prone to future breakouts. External triggers such as environmental stress, skincare habits, and lifestyle factors can further amplify this inflammatory state, causing acne to fluctuate over time.
The skin barrier plays a critical role in long-term acne control. If the barrier is compromised—whether by overuse of harsh treatments or inconsistent routines—the skin becomes more susceptible to irritation and increased oil production. This can create a cycle in which attempts to aggressively treat acne actually contribute to its persistence. Maintaining barrier health through consistent, balanced skincare is therefore essential for ongoing management.
Treatment itself is typically divided into two phases: active treatment and maintenance. Active treatment focuses on reducing existing lesions using ingredients such as benzoyl peroxide, salicylic acid, or retinoids. Maintenance, however, is equally important and involves continued use of appropriate products at a lower intensity to prevent new breakouts from forming. Without this maintenance phase, the underlying processes that drive acne can gradually reestablish themselves.
Acne should be understood as a chronic, relapsing condition rather than a problem that can be permanently cured with a single intervention. Effective management involves long-term consistency, adaptation of routines based on the skin’s needs, and realistic expectations about fluctuations. While many individuals can achieve significant and lasting improvement, occasional breakouts may still occur. For persistent or severe acne, ongoing guidance from a qualified dermatologist can help maintain control while minimizing irritation and supporting overall skin health.