Video 1
Video 2
Video 3
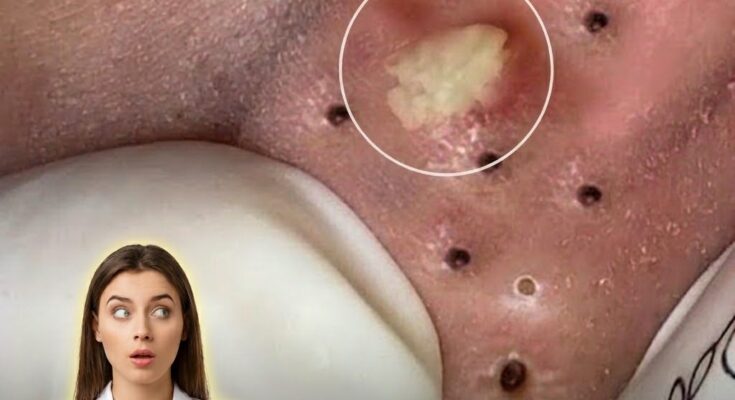
Dairy consumption has been studied for its potential role in acne development, particularly through its influence on hormonal signaling pathways that regulate sebum production and follicular activity. Milk and other dairy products naturally contain bioactive molecules, including hormones and growth factors, that may stimulate insulin and insulin-like growth factor-1 (IGF-1). Elevated IGF-1 levels are associated with increased sebum production and enhanced keratinocyte proliferation, both of which contribute to clogged pores and the formation of comedones such as blackheads and whiteheads. These processes can create an environment where acne-causing bacteria thrive, leading to inflammation and visible breakouts.
The relationship between dairy and acne is not uniform across all individuals, as genetic predisposition, baseline hormone levels, and overall diet can influence how the skin responds. Some people may notice increased breakouts when consuming skim milk in particular, which has been more strongly associated with acne in observational studies. This may be due to processing differences or the relative concentration of certain bioactive compounds. Additionally, diets high in refined carbohydrates and sugars can amplify insulin signaling, potentially compounding the effects of dairy on acne-prone skin. Environmental factors, stress, and inconsistent skincare routines may further interact with these internal triggers, making it difficult to isolate a single cause.
From a skincare perspective, managing acne linked to dietary factors often involves addressing the downstream effects on the skin rather than relying solely on dietary elimination. Ingredients such as salicylic acid may help unclog pores by promoting exfoliation within the follicle, while benzoyl peroxide is commonly used to reduce acne-causing bacteria and inflammation. Topical retinoids can support normalization of skin cell turnover, helping to prevent the formation of new comedones. Niacinamide may also be beneficial for regulating oil production and supporting the skin barrier, which can become compromised in acne-prone individuals. In more persistent cases, dermatological treatments such as prescription retinoids or hormonal therapies may be considered under professional guidance.
It is important to recognize that eliminating dairy does not guarantee improvement in acne, and overly restrictive diets may lead to nutritional imbalances if not carefully managed. Instead, a more measured approach is often recommended, where individuals monitor their skin’s response to dietary changes over time while maintaining a consistent, evidence-based skincare routine. Because acne is a multifactorial condition involving hormones, sebum production, follicular keratinization, and inflammation, long-term management typically requires a combination of lifestyle awareness and targeted treatment. Consulting a qualified healthcare professional may be helpful for those experiencing persistent or severe breakouts to ensure that both dietary and dermatological factors are appropriately addressed