Video 1
Video 2
Video 3
Video 4
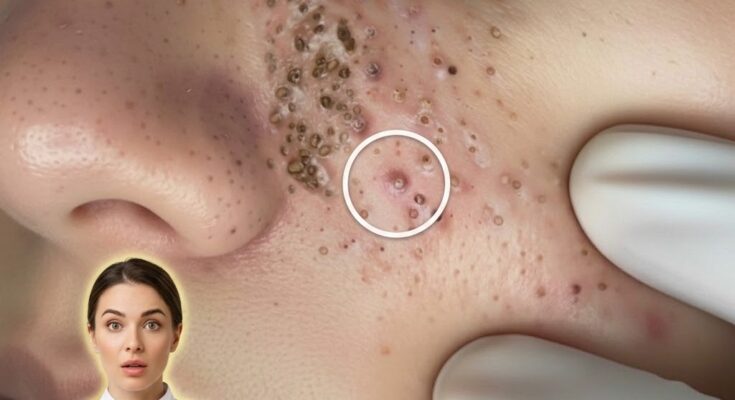
Dry acne-prone skin presents a unique challenge because it involves two seemingly opposing conditions: reduced moisture levels alongside the formation of clogged pores and inflammation. Acne develops when excess sebum, dead skin cells, and debris accumulate داخل the hair follicle, leading to comedones such as blackheads and whiteheads. Even in dry skin types, follicular keratinization can become irregular, causing dead skin cells to build up instead of shedding normally. When the skin barrier is compromised, which is common in dry skin, inflammation can increase and make acne lesions more persistent and sensitive.
Several contributing factors can worsen both dryness and breakouts simultaneously. Overuse of strong acne treatments such as benzoyl peroxide or high-strength retinoids may strip the skin and disrupt barrier function, leading to increased transepidermal water loss. In response, the skin may produce more oil in an attempt to compensate, which can further clog pores. Environmental factors such as low humidity, air conditioning, and harsh cleansers also play a role in weakening the barrier. Hormonal fluctuations and genetic predisposition can influence sebum production and skin cell turnover, making some individuals more prone to this combination of dryness and acne.
An effective routine for dry acne-prone skin focuses on balancing gentle treatment with barrier support. Cleansing should be mild and non-foaming, using a hydrating cleanser that removes excess oil and impurities without stripping essential lipids. Ingredients such as ceramides and glycerin are often recommended because they help maintain hydration while preserving barrier integrity. Treatment steps may include low-concentration salicylic acid, which can penetrate pores and help reduce comedones without excessive irritation, or carefully introduced retinoids that normalize cell turnover. These should be used gradually to avoid worsening dryness.
Moisturizing is a critical step that should not be skipped, even in acne-prone skin. Lightweight, non-comedogenic moisturizers containing ingredients like hyaluronic acid, niacinamide, and ceramides can help restore hydration and reduce inflammation. Niacinamide, in particular, may help regulate oil production while supporting the skin barrier. Sunscreen is also essential, as UV exposure can worsen inflammation and delay healing, especially when using active treatments.
For individuals with persistent or moderate acne, dermatological options may be considered. Prescription retinoids, azelaic acid, or combination therapies can be tailored to manage acne while minimizing irritation. In some cases, adjusting treatment frequency rather than increasing strength is more beneficial for maintaining balance in dry, sensitive skin.
It is important to maintain realistic expectations, as improvements in acne and skin hydration typically take several weeks to become noticeable. Overloading the skin with multiple active ingredients can worsen both dryness and breakouts, so a simplified and consistent routine is often more effective. Monitoring how the skin responds and making gradual adjustments can help prevent barrier damage. Consulting a qualified dermatologist is recommended for persistent or severe cases to ensure that treatment is both safe and appropriate.