Video 1
Video 2
Video 3
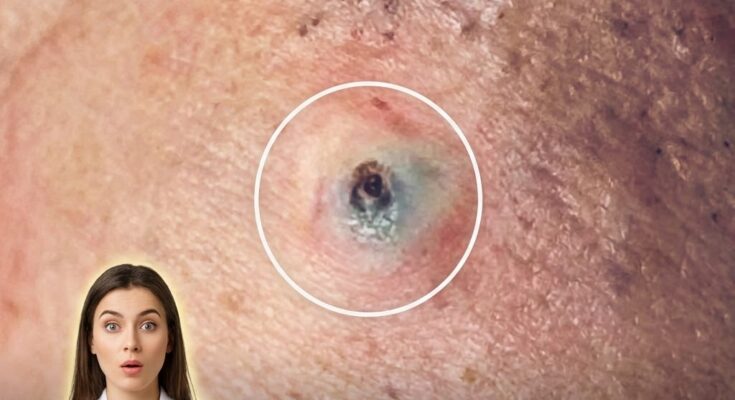
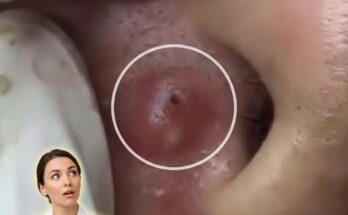
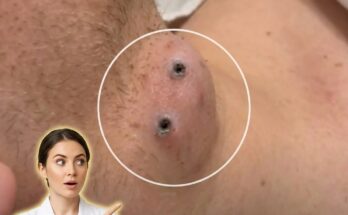
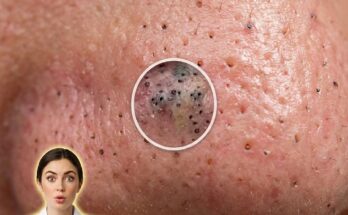
Sleeping with makeup directly affects the biology of pores by interfering with the normal function of the pilosebaceous unit, where sebum is produced and expelled through hair follicles. Throughout the day, the skin accumulates sebum, dead skin cells, environmental pollutants, and cosmetic products. When makeup is left on overnight, this mixture can settle into pores and contribute to follicular occlusion. This process promotes the formation of microcomedones, which are the earliest stage of acne lesions and can develop into blackheads, whiteheads, or inflammatory acne over time.
Makeup products, particularly those with occlusive or heavy formulations, may combine with natural oils and keratinized skin cells to thicken the material inside pores. This can disrupt normal shedding of skin cells, a process known as desquamation, and lead to buildup within the follicle. As pores become congested, oxygen levels decrease, creating an environment that may support the proliferation of acne-associated bacteria such as Cutibacterium acnes. This can further contribute to inflammation, redness, and the progression of acne lesions.
Several contributing factors can increase the likelihood of pore congestion when sleeping with makeup. Individuals with oily skin or higher sebum production may be more prone to clogged pores because excess oil can bind more easily with residual makeup. Hormonal fluctuations can also increase sebum output, compounding the effect. Environmental exposure, including pollution and humidity, may add additional particles to the skin surface, which become trapped under makeup layers. In addition, repeated neglect of nighttime cleansing can weaken the skin barrier, making the skin more reactive and prone to breakouts.
From a skincare perspective, consistent and gentle cleansing in the evening is commonly recommended to reduce pore blockage. Cleansers containing ingredients such as salicylic acid may help dissolve excess oil and penetrate into pores, supporting the removal of debris. Retinoids are often used to regulate skin cell turnover and reduce the formation of comedones over time. Benzoyl peroxide may help limit bacterial growth in acne-prone skin, while niacinamide can support barrier function and reduce inflammation. Choosing non-comedogenic makeup products may also reduce the likelihood of pore clogging, although proper removal remains essential regardless of product type.
Professional treatments may be considered when persistent clogged pores or acne develop. Dermatological options such as chemical peels, topical prescriptions, or comedone extraction can help manage more resistant cases. These approaches are typically tailored based on skin type, acne severity, and individual tolerance.
While occasional lapses in removing makeup may not immediately result in acne for everyone, regular overnight buildup can gradually contribute to clogged pores and skin imbalance. Maintaining a consistent cleansing routine, using appropriate skincare ingredients, and supporting the skin barrier are important for long-term skin health. Individuals experiencing ongoing breakouts or worsening acne may benefit from consulting a qualified dermatologist for personalized evaluation and treatment guidance.