Video 1
Video 2
Video 3
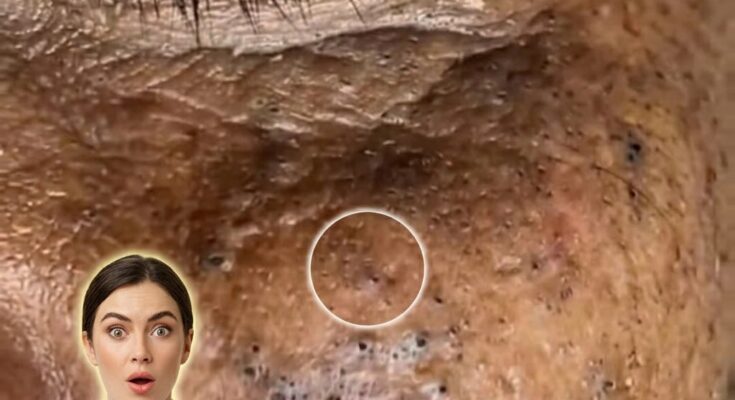
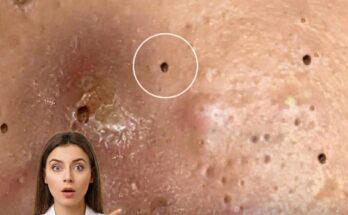
Comedones are the earliest visible form of acne and develop when hair follicles, commonly referred to as pores, become clogged with a combination of sebum and dead skin cells. Under normal conditions, skin cells within the follicle shed in a controlled manner and rise to the surface. In acne-prone skin, this process becomes disrupted, leading to a buildup of keratinized cells that mix with oil and form a plug inside the pore. This process, known as follicular keratinization, is a central mechanism in the formation of comedonal acne.
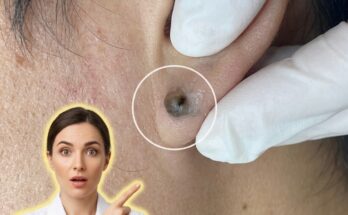
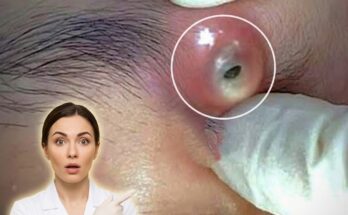
There are two primary types of comedones, defined by whether the pore remains open or closed at the surface. Open comedones, often called blackheads, occur when the clogged material is exposed to air and undergoes oxidation, giving it a darker appearance. Closed comedones, or whiteheads, form when the pore opening is covered by a thin layer of skin, trapping the contents beneath the surface. Both types represent non-inflammatory acne lesions, although they can progress into inflamed pimples if bacteria proliferate within the blocked follicle.
Several biological and environmental factors can contribute to the formation of comedones. Increased sebum production, often influenced by hormonal changes, creates a lipid-rich environment that promotes clogging. At the same time, impaired shedding of skin cells causes them to accumulate rather than exit the pore efficiently. External factors such as the use of comedogenic skincare or cosmetic products, exposure to pollution, and inadequate cleansing may also contribute to buildup within pores. In some individuals, genetic predisposition can make follicles more prone to blockage.
The development of comedones is also closely linked to the skin barrier and microbiome. When the barrier is compromised, irritation and inflammation can alter normal cell turnover and oil regulation, indirectly increasing the likelihood of clogged pores. Additionally, shifts in the balance of skin bacteria may create conditions that favor acne progression, especially when comedones become inflamed.
Managing comedones typically focuses on normalizing skin cell turnover and reducing excess oil while maintaining barrier health. Ingredients such as salicylic acid are commonly used because they are oil-soluble and can penetrate into the pore to help dissolve debris. Retinoids are also widely recommended, as they support more regular shedding of skin cells and help prevent the formation of new blockages. Niacinamide may help regulate sebum production and reduce inflammation, making it a supportive ingredient in many routines.
Professional treatments may be considered when comedones are persistent or widespread. Dermatologists may perform extractions to remove clogged material or recommend chemical peels to promote exfoliation at a deeper level. Prescription-strength retinoids or other medications may also be used to improve long-term outcomes. However, these approaches are typically combined with consistent daily skincare to maintain results.
It is important to understand that comedonal acne develops over time and does not resolve immediately. Improvements often require several weeks of consistent treatment, and overuse of strong products can lead to irritation that may worsen the condition. A balanced approach that targets clogged pores while preserving the skin barrier is generally the most effective strategy for managing and preventing comedones.