Video 1
Video 2
Video 3
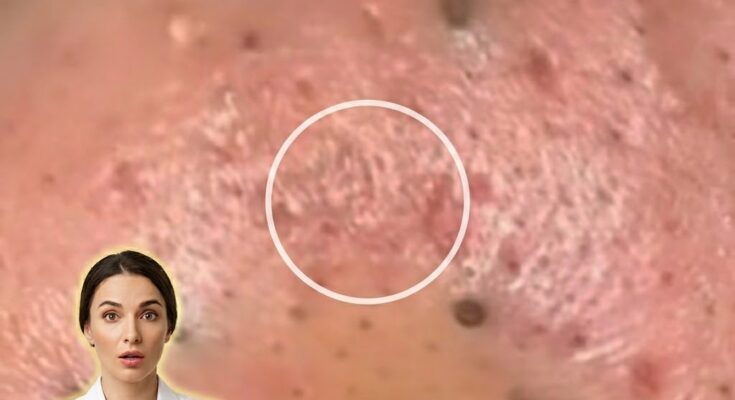
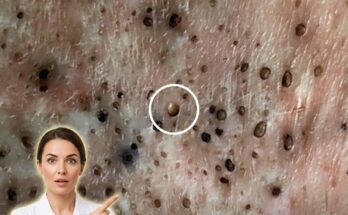
Acne formation is closely linked to the activity of skin-resident bacteria, particularly Cutibacterium acnes, a microorganism that naturally lives within the pores. Under normal conditions, this bacterium exists as part of the skin’s microbiome and does not cause harm. However, when excess sebum production and abnormal shedding of skin cells lead to clogged pores, an oxygen-poor environment develops inside the follicle. This environment allows C. acnes to proliferate more rapidly. As the bacteria multiply, they break down sebum into inflammatory byproducts, which can trigger the immune system and contribute to redness, swelling, and the formation of inflamed acne lesions such as papules and pustules.
The role of bacteria in acne is not isolated but interacts with several underlying biological processes. Increased sebum production, often influenced by hormonal fluctuations, provides a nutrient-rich environment that supports bacterial growth. At the same time, follicular keratinization, where dead skin cells accumulate and block pores, creates the enclosed space necessary for bacterial overgrowth. Genetics may also influence how the immune system responds to C. acnes, meaning some individuals are more prone to inflammation than others. Additionally, external factors such as occlusive skincare products, environmental pollution, and inconsistent cleansing habits can further contribute to pore congestion and microbial imbalance.
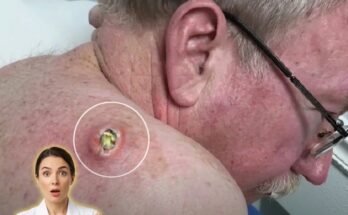
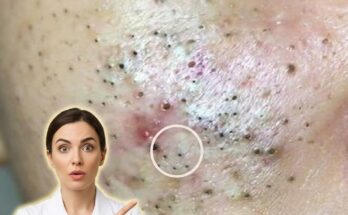
Inflammation driven by bacterial activity plays a central role in the progression from non-inflammatory lesions like blackheads and whiteheads to more severe forms of acne. When the immune system detects bacterial overgrowth, it releases inflammatory mediators that can damage surrounding tissue. This process not only leads to visible breakouts but may also increase the risk of post-inflammatory hyperpigmentation or scarring, particularly if lesions are manipulated or left untreated. Maintaining the balance of the skin barrier is therefore important, as excessive irritation or overuse of harsh treatments can worsen inflammation and disrupt the microbiome further.
Treatment strategies often focus on reducing bacterial overgrowth while also addressing other contributing factors such as oil production and clogged pores. Ingredients like benzoyl peroxide are commonly used because they introduce oxygen into the pore, making it less favorable for C. acnes survival. Salicylic acid may help by exfoliating داخل the pore lining, reducing blockages that trap bacteria. Retinoids are often recommended to normalize skin cell turnover, preventing the formation of comedones where bacteria can thrive. Niacinamide may support the skin barrier and help reduce inflammation, which can be beneficial in managing acne-prone skin. In more persistent or moderate to severe cases, dermatologists may recommend topical or oral medications that target both bacterial activity and inflammation more directly.
While targeting bacteria is an important aspect of acne care, it is not a complete solution on its own. Acne is a multifactorial condition, and long-term improvement typically requires a balanced approach that considers sebum regulation, pore health, and skin barrier support. Overuse of antibacterial treatments may lead to dryness or irritation, which can paradoxically worsen breakouts. Consistent, gentle skincare routines combined with appropriate active ingredients tend to provide more sustainable results.
Realistic expectations are essential when managing acne related to bacterial activity. Improvements often take several weeks as the skin undergoes its natural renewal cycle. Not all treatments work the same for everyone, and some trial and adjustment may be necessary. Individuals experiencing persistent, painful, or scarring acne are generally advised to seek guidance from a qualified dermatology professional to ensure that treatment is both effective and appropriate for their skin type and condition.