Video 1
Video 2
Video 3
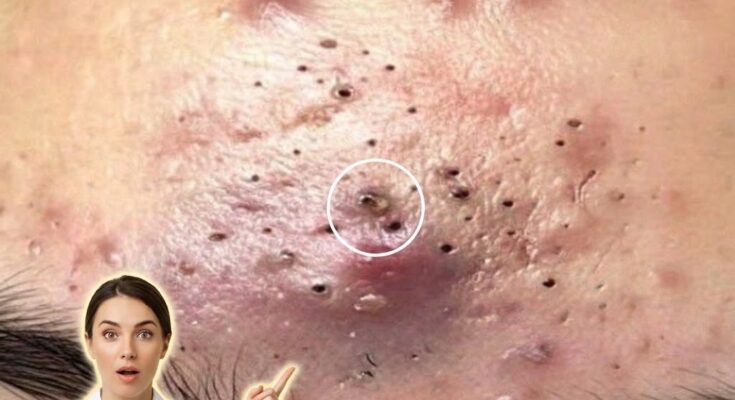
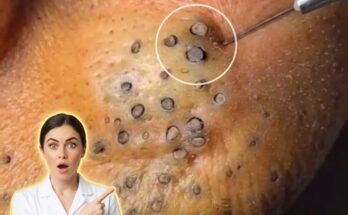
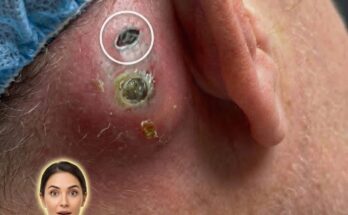
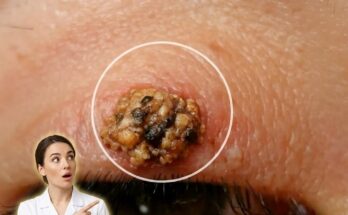
Acne-prone skin is influenced by a combination of biological processes that tend to persist over time rather than resolve quickly. At the core of acne development is the interplay between sebum production, follicular keratinization, microbial activity, and inflammation. Sebaceous glands produce oil to maintain skin hydration, but in acne-prone individuals, this production may be excessive or more reactive to hormonal signals. At the same time, the lining of the hair follicle can shed dead skin cells unevenly, leading to clogged pores. These blockages form comedones such as blackheads and whiteheads, which can then become inflamed when bacteria proliferate within the pore. Effective long-term management focuses on regulating these underlying processes rather than addressing only visible breakouts.
Hormonal fluctuations are one of the most significant contributors to ongoing acne activity. Androgens can stimulate sebaceous glands, increasing oil production and making pores more prone to congestion. Genetic predisposition also plays a role, as some individuals naturally produce more sebum or have a tendency toward irregular skin cell turnover. Environmental factors such as humidity, pollution, and occlusive skincare or cosmetic products can further contribute to clogged pores. In addition, inconsistent skincare habits, including over-cleansing or using harsh products, may weaken the skin barrier and lead to increased irritation and rebound oil production. These combined influences explain why acne often requires consistent, long-term management rather than short-term solutions.
A sustainable skincare approach typically includes ingredients that target multiple aspects of acne formation. Retinoids are commonly recommended because they help normalize skin cell turnover and reduce the formation of comedones over time. Salicylic acid, a beta hydroxy acid, is oil-soluble and can penetrate into pores to help clear excess sebum and debris. Benzoyl peroxide is often used for its antibacterial properties and its ability to reduce inflammation associated with active breakouts. Niacinamide may support the skin barrier while also helping to regulate oil production and reduce redness. Gentle cleansing and the use of non-comedogenic moisturizers are also important to maintain barrier function and prevent irritation that can worsen acne.
For individuals with persistent or more severe acne, professional treatments may be considered as part of long-term management. Dermatologists may recommend prescription-strength retinoids, topical or oral antibiotics for inflammatory acne, or hormonal therapies in cases where androgen activity is a significant factor. Procedures such as chemical peels or light-based therapies may also be used to complement topical treatments, particularly for managing clogged pores and improving overall skin texture. These approaches are typically tailored to the individual and adjusted over time based on response and tolerance.
Long-term management of acne-prone skin requires patience and consistency, as visible improvements often develop gradually over weeks to months. It is important to avoid frequent changes in products, as this can disrupt the skin and make it difficult to assess what is effective. While many treatments may help reduce breakouts and improve skin clarity, acne can still fluctuate due to internal and external factors. Maintaining realistic expectations and focusing on steady control rather than quick results can lead to more sustainable outcomes. Individuals experiencing persistent or severe acne are encouraged to seek guidance from a qualified healthcare professional to ensure safe and appropriate treatment strategies.