Video 1
Video 2
Video 3
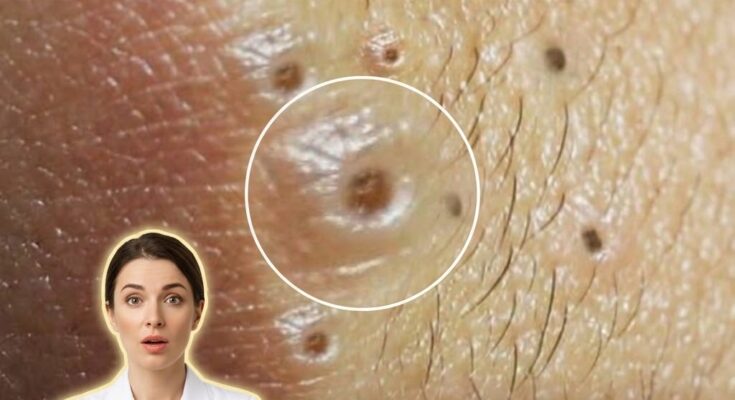
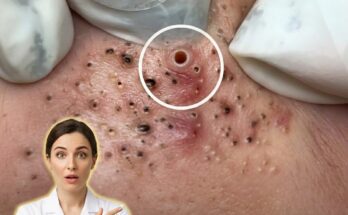
Harsh scrubs may irritate acne-prone skin because they disrupt the skin’s barrier and aggravate the underlying processes involved in acne formation. Acne develops when excess sebum combines with dead skin cells inside the pore, leading to clogged follicles known as comedones. Inflammatory acne can follow when bacteria proliferate within these blocked pores. Physical scrubs, especially those with rough or uneven particles, can create microscopic tears in the skin’s surface. This mechanical damage may trigger inflammation, weaken the skin barrier, and increase transepidermal water loss, all of which can worsen the environment that allows acne to persist.
The skin barrier plays a central role in maintaining balance, particularly for individuals with oily or acne-prone skin. When harsh scrubbing strips away natural lipids, the skin may respond by producing more oil to compensate for the loss of moisture. This rebound increase in sebum can contribute to further pore congestion and the formation of blackheads and whiteheads. At the same time, irritation caused by aggressive exfoliation may stimulate inflammatory pathways, making existing breakouts appear more red, swollen, and sensitive. Repeated friction can also spread bacteria across the skin’s surface, potentially leading to new breakouts in previously unaffected areas.
Certain skincare habits and environmental factors can amplify the negative effects of harsh scrubs. Over-cleansing, frequent exfoliation, and combining physical scrubs with strong active ingredients such as benzoyl peroxide or retinoids may compound irritation. Individuals living in humid or polluted environments may already experience increased oil production and clogged pores, making their skin more vulnerable to barrier disruption. Genetic predisposition and hormonal fluctuations can further influence how reactive the skin becomes when exposed to mechanical stress.
In many cases, gentler and more controlled exfoliation methods are preferred for acne-prone skin. Chemical exfoliants such as salicylic acid, a beta hydroxy acid, are commonly used because they can penetrate into the pore lining and help dissolve excess oil and debris without the need for abrasive friction. Retinoids may also support normal skin cell turnover and reduce the formation of comedones over time. Ingredients like niacinamide can help regulate oil production and support barrier repair, which may reduce sensitivity and improve overall skin resilience. Dermatologists often recommend limiting exfoliation frequency and choosing formulations designed specifically for acne-prone or sensitive skin.
Professional treatments may be considered for persistent or severe cases. Dermatological procedures such as chemical peels or extraction performed under controlled conditions can address clogged pores while minimizing unnecessary trauma to the skin. These approaches are typically tailored to the individual’s skin type and acne severity, reducing the risk of irritation associated with improper at-home exfoliation.
Realistic expectations are important when managing acne-prone skin. While exfoliation can be beneficial, more aggressive methods do not necessarily lead to better results and may instead delay healing by perpetuating inflammation. A balanced approach that prioritizes barrier protection, consistent use of appropriate active ingredients, and gradual adjustments to skincare routines is generally more effective over time. Individuals experiencing ongoing irritation or worsening acne may benefit from consulting a qualified dermatology professional for personalized guidance.