Video 1
Video 2
Video 3
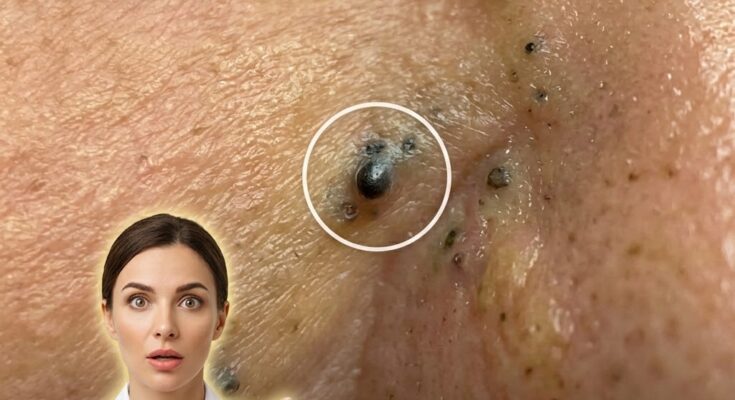
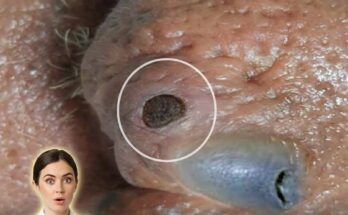
Masks and other forms of occlusion can influence acne development through a combination of mechanical and biological effects on the skin. Occlusion refers to the trapping of heat, moisture, oil, and sweat against the skin surface. When the skin is covered for prolonged periods, the microenvironment within the pores changes. Increased humidity softens the outer layer of the skin, which can alter normal shedding of dead skin cells. At the same time, sebum production may remain active, leading to a mixture of oil and keratin that can accumulate within hair follicles. This process contributes to follicular keratinization and the formation of clogged pores, which may later develop into blackheads, whiteheads, or inflammatory acne lesions.
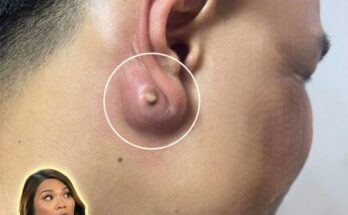
Friction and pressure from masks can further aggravate this process. Repeated rubbing against the skin, especially along the cheeks, chin, and jawline, can disrupt the skin barrier and trigger localized inflammation. This mechanical stress may stimulate increased oil production and worsen existing comedones. In some cases, this combination of friction and occlusion is referred to as acne mechanica. Environmental conditions, such as hot and humid climates, can intensify these effects by increasing sweat production. Sweat, when trapped under a mask, mixes with oil and debris, further contributing to pore congestion. Individual factors, including naturally oily skin, hormonal fluctuations, and genetic predisposition, may also influence how strongly someone reacts to prolonged occlusion.
Skincare habits play a significant role in either mitigating or worsening mask-related breakouts. Using heavy or occlusive skincare products under a mask may increase the likelihood of clogged pores, particularly if formulations are not suited for acne-prone skin. In contrast, lightweight, non-comedogenic moisturizers can help maintain the skin barrier without contributing to congestion. Gentle cleansing is important to remove accumulated oil, sweat, and environmental impurities, but overwashing or using harsh cleansers may disrupt the barrier and lead to increased irritation. Ingredients such as salicylic acid are commonly used to penetrate pores and help dissolve excess oil and debris, while retinoids may support normalized skin cell turnover. Benzoyl peroxide may help reduce acne-causing bacteria, and niacinamide is often included to support oil regulation and reduce visible redness.
Adjustments in daily habits may also help reduce the impact of occlusion. Regularly changing or washing reusable masks can minimize the buildup of bacteria, oil, and residue. Choosing breathable, soft fabrics may reduce friction, while ensuring a proper fit can limit unnecessary pressure on the skin. Avoiding heavy makeup under masks may also decrease the risk of pore blockage, particularly in individuals prone to comedonal acne.
Although mask-related breakouts can be frustrating, they are typically manageable with consistent and balanced skincare. Improvements often take time, as acne treatments generally require several weeks to show visible results. If breakouts become persistent, severe, or resistant to over-the-counter approaches, consultation with a qualified dermatologist is recommended. Professional guidance may include prescription treatments or tailored skincare strategies based on individual skin type and acne severity.